Home Healthcare
Home healthcare may be a service provided by an acute care facility or it may be a service provided by an agency that specializes in home healthcare (Fig. 3-1). Home healthcare focuses on the return of health using a recuperative environment that is familiar to the client. Services in the home often include intravenous medications, respiratory care, and wound care. Visits by the nurse may be one or more times per day, weekly, or monthly, as prescribed by the healthcare provider. The family or a significant other is often the main caregiver, with the nurse assisting using assessment/data-gathering skills, specialized training (e.g., in diabetes), or follow-up care. Nurses provide the specialized knowledge to treat diseases and disorders, or postoperative therapies.
Key Concept Many individuals prefer to be cared for at home. Home care is also less expensive than hospitalization. Individuals often have family or friends who can assist in their care. Home health nursing and hospice care have greatly enhanced the quality of healthcare available in the home.
Special Considerations : LIFESPAN
The frail or confused elderly may have difficulty managing at home without assistance. Nurses, discharge planners, and physicians work as a team to provide safe and adequate care to those individuals living at home. Home health agencies and social services can assist in discharge planning and make arrangements for home care or public health nursing visits.
Hospice
Hospice care specializes in the care of the terminally ill. This service also may be part of the services available from an acute care facility or a separate private agency. Hospice care and home care share a similar nursing objective: taking care of a client in a home environment versus a traditional hospital setting. However, they are two different specialty areas of care. Hospice care focuses on the transition from life to death and works with the client, family, and significant others.
Respite Care
Healthcare services have recognized the need for respite care. Respite care provides part-time supervision of clients who have chronic conditions. Family or friends who are the primary caregivers for children and adults with serious, chronic medical conditions or mental illness need respite care. The client may be taken to a facility for part of the day. The client receives supervised care and has an opportunity for socialization outside the home. The caregiver has a chance to be relieved of the exhausting and constant responsibility and stress of caring for someone 24 hours a day.
Telehealth
Telehealth is a service that is relatively new and growing. The term telehealth refers to the ability to access a nurse or physician via telephone or computer audio/video link. Nurses can communicate and assist clients in numerous ways using distance communication modes. Frequent contact with clients helps to increase medication compliance and helps healthcare providers recognize potential problems before they become acute problems. Thus, unscheduled visits to the physician, the emergency room, and rehospitalization are decreased. Physicians use telehealth to contact other physicians or specialty facilities. Rural communities find the immediate contact with physician specialists a great asset in client care. This concept is discussed in more detail later in this text.
Extended Care Facilities
Some facilities admit clients for longer periods of time than is common in acute care hospitals. These extended care facilities (ECFs) include nursing homes, inpatient rehabilitation centers, inpatient treatment centers for chemical dependency, and facilities for chronic mental healthcare. Some facilities are attached to a general hospital; others are free-standing. More emphasis is being placed on returning people to their homes or other community-based living facilities as quickly as possible. Thus, the population in long-term care facilities is changing.
The federal government divides nursing homes into two categories: a skilled nursing facility or an intermediate care facility. The skilled nursing facility (SNF) provides 24-hour nursing care under the supervision of a registered nurse (RN). The intermediate care facility (ICF) provides 24-hour service from nursing assistants under the supervision of an LPN/LVN, with an RN as a consultant. Many rules and regulations apply to nursing homes. The employment opportunities for nurses continue to grow in this area.
Community Health Services
Community health services provide care for individuals and families within a specific area, such as a neighborhood, a small town, or a rural county. The costs of in-hospital medical care, along with governmental limits and regulations, have forced many people to be cared for in the community, rather than in a hospital.
One type of community health service is the public health service. Public health departments offer immunizations, well-baby checks, and treatment for specific diseases, such as tuberculosis or sexually transmitted diseases (STDs).
Community health clinics offer low-cost healthcare services to the public. Prenatal and pediatric care, diabetic care, and general medical-surgical ambulatory care services may be offered by community health clinics.
Independent living facilities may provide care for a small number of individuals in a house located in a community neighborhood. These facilities provide a stable, home-like environment for mentally challenged individuals, while still providing some degree of supervision.
Healthcare in School and Industry
Most school systems provide some healthcare services for students, particularly those with disabilities. A nurse may be on duty full time, or divide time among several schools. In addition to assisting ill children or children in emergencies, the nurse provides preventive care by performing regular assessments, teaching, screening for common disorders, supervising the administration of immunizations and medications, and providing health counseling.
Children with special physical challenges receive more intensive nursing care, sometimes on a one-to-one basis. An increasing number of school systems operate or house school-based comprehensive clinics to provide total healthcare to students.
Industries in which machinery is operated usually employ a nurse for health promotion and interventions. Teaching is part of the nurse’s responsibility, and prevention of accidents is a major goal. The industrial nurse often serves as liaison between the industry and the Occupational Safety and Health Administration (OSHA).
QUALITY ASSURANCE
Quality of care has become a major issue for both consumers and providers of healthcare. Quality assurance (QA) is defined as a pledge to the public that healthcare services will provide optimal achievable goals and maintain standard excellence in the services rendered.
Hospital Accreditation
Just as your nursing program can be accredited, a hospital or other healthcare facility also can be accredited. Accreditation implies that the facility has met rigid, minimal standards of service to the client and the community. The agency that assigns this recognition to hospitals is called the Joint
Commission (formerly known as the Joint Commission for Accreditation of Healthcare Organizations or JCAHO). Other facilities have similar accreditation processes.
The Joint Commission has established rigid standards for an ongoing quality assurance program in hospitals, as well as for community health centers, home care agencies, and various levels of extended care facilities. The Joint Commission requires objective and systematic monitoring and evaluation of the quality and appropriateness of client care. The quality assurance procedure requires healthcare facilities to identify what they mean by “quality” and to define their evaluation methods.
NCLEX Alert When reading an NCLEX question, look for the option that suggests the best possible action.
Do not confuse the best NCLEX response with an action or shortcut that you might have witnessed while working in a similar situation. Correct nursing options should consider the safety of a situation, the quality of care, and the priorities of nursing care.
Components of Quality Care
Quality management requires that healthcare services be well planned and delivered in a manner that ensures good care. Adequate staff and support services, such as nursing care, must be available.
Quality control and quality assurance focus on delivery of care. The process of care is important, as is the outcome. Process relates to how care is given. Outcome relates to the result, which is also known as outcome-based care.
Nurse accountability, which involves the delivery and accurate documentation of quality care, is vital. Healthcare facilities and agencies have contiguous (or continuous) quality improvement (CQI) committees that monitor the quality of ongoing care.
Standards for Quality Assurance
Each healthcare facility establishes individual standards of quality to guide the nursing staff in providing care. In general, these standards include:
• Standards of nursing practice: Procedures used in the delivery of care, the hospital policy book, textbooks, and other references. Sometimes the term nursing protocol is used. Standards of nursing practice focus on the caregiver, the nurse, and on the nursing process (see Unit 6).
• Standards of client/patient care: Activities determined by client expectations or by personal standards of care. What did the client expect? How well did nursing care meet the client’s expectations? Standards of client care focus on the recipient of care, the client. The client participates in developing the nursing care plan. (The “case manager” is responsible for making sure the client’s care is planned and carried out appropriately.)
• Standards of performance: How well the nurse performs, as compared with a job description. How well you meet standards of performance as a nursing student will change as you progress through the program. As you become more experienced, you will be expected to provide more complex nursing care.
The nursing audit committee or CQI committee evaluates care given to clients. Peer review allows nurses to constructively critique each other.
Client Representatives or Advocates
Many hospitals have initiated the position of client (patient) representative, advocate, liaison, or ombudsperson. This person’s role is to act as consumer advocate. As an advocate, the ombudsperson assists the client and family by resolving concerns or problems. The goal is to focus on client care, needs, and concerns, not the problems that may be encountered during the hospital admission.
Client representatives often help clients and their families find needed services. They listen and answer questions. Representatives can help families find housing, restaurants, parking, child care, or chaplain services. During hospitalization, clients have the right to contact their representatives if they have a problem or concern. Each individual is informed about and receives a copy of the Patient’s Bill of Rights.In preparation for discharge, the advocate can make sure the family knows where to purchase needed supplies and medications. The nursing case manager has overall responsibility for the client’s care. The advocate assists as needed.
ORGANIZATION AND OWNERSHIP OF HEALTHCARE FACILITIES
Hospital Organization
Hospitals are almost always governed by a board of directors or trustees, or in the case of a university hospital, by a board of regents. This board appoints the administrators of the hospital. The hospital administrator in turn develops an organizational structure. Box 3-2 lists some of the numerous administrative individuals who are necessary in a modern healthcare facility.
BOX 3-2. Administrative Individuals in a Healthcare Facility
|
Each healthcare facility requires numerous trained individuals working together: The chain-of-command binds the hospital team members into organized units. |
|
♦ Chief Executive Officer |
|
♦ Medical Staff and Services |
|
♦ Nursing Staff and Services |
|
♦ Financial Officer |
|
♦ Quality Assurance |
|
♦ Engineering and Maintenance |
|
♦ Environmental Services |
|
♦ Safety Officer |
|
♦ Medical Records |
|
♦ Purchasing |
|
♦ Dietitian |
|
♦ Human Resources |
|
♦ Billing and Accounts |
|
♦ Infection Control |
|
♦ Education |
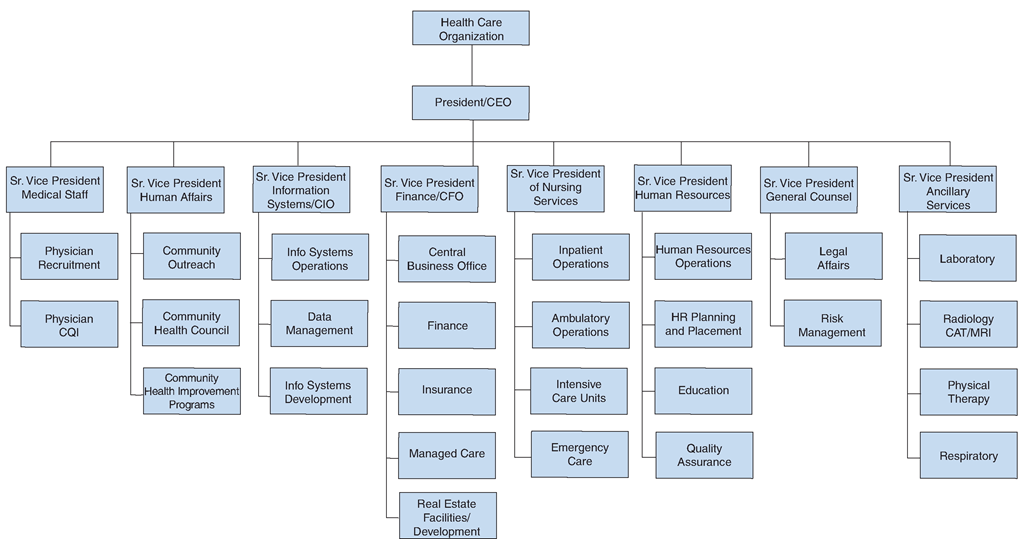
It is important that the student and future employee learn the administrative structure of each healthcare facility. All facilities follow a chain-of-command or organizational reporting system. It is critical that the nurse use the appropriate system for communication (i.e., chain-of-command) with peers and supervisors. Figure 3-2 gives an overview of an administrative organization in a typical healthcare facility.
Key Concept While you are in your nursing program, your chain-of-command begins with your instructor Problems, concerns, or issues should first be directed to your immediate supervisor (instructor). Each program will have a designated chain-of-command for students to follow.
Teamwork is a critical component of healthcare. To provide care, members of the healthcare team collaborate in their assessments, planning, and delivery of care. Team members communicate with one another and with clients so that services are neither duplicated nor omitted. Their goal is to help clients maintain wellness. When they find problems, team members focus their energies on restoring clients to health. As a nurse or a nursing student, you are part of the team providing healthcare.
Hospital Ownership and Funding
In addition to types of clients served, healthcare facilities are classified in relation to ownership and funding structure. These lines are becoming blurred, as mergers occur between various types of hospitals.
Governmental Ownership
Governmental, public, or official hospitals are nonprofit organizations that are owned and operated by local, state, or federal units of government. These governmental agencies are also called official hospitals. Box 3-3 provides some examples.
Private Ownership
Private or voluntary hospitals are owned and operated by individuals or by groups, such as churches, labor unions, and fraternal organizations. These hospitals may be established as for-profit or not-for-profit organizations.
For-Profit Versus Not-for-Profit
A further classification of hospitals relates to distribution of their profits:
• Proprietary, investor-owned, or for-profit hospitals are those in which profits are returned to shareholders. Very few such hospitals exist today. Many nursing homes, however, fall into this category.
• Not-for-profit hospitals constitute the majority of all hospitals. In the not-for-profit hospital, profits are returned to the funding agency, and are used for improvements to the facility, added equipment, and other related costs.
FIGURE 3-2 • An overview of administrative organization in a typical healthcare facility.
BOX 3-3. Types of Ownership of Healthcare Facilities
|
Profit Oriented—Proprietary |
|
♦ Individual ♦ Partnership ♦ Corporation |
|
Nonprofit—Voluntary |
|
♦ Church Associated (e.g., Loma Linda University Medical Center) ♦ Private-School Associated ♦ Foundation Associated (e.g., Shriner’s Hospitals) |
|
Nonprofit—Government |
|
♦ Federal (e.g., Veterans Administration, active duty military hospitals) ♦ State (e.g., university hospital) ♦ County (e.g., city or county hospital) ♦ City (e.g., city or county hospital) ♦ City-County (e.g., city or county hospital) |