Learning Objectives
1. Compare the education and level of practice between registered and practical nurses.
2. Explain the various types of educational programs that lead to licensure.
3. Identify the standards of the National Federation of Licensed Practical Nurses in relationship to each of the following: education, legal status, and practice.
4. Differentiate between permissive and mandatory licensure.
5. Discuss the reasons for a nurse to seek licensure.
6. Identify the importance of the nurse’s pledge.
7. Explain the importance of nursing theory and how a theoretical framework helps nurses in their learning, understanding, and practice.
8. List the roles of today’s nurse, briefly explaining each one.
9. Discuss the importance of nurses projecting a professional image.
10. Discuss the goals of at least three nursing organizations and state at least two reasons why a student or a licensed nurse should join a professional organization.
IMPORTANT TERMINOLOGY
|
accreditation |
licensure |
reciprocity |
|
advanced practice nurse |
mandatory licensure |
theoretical framework |
|
approval |
Nurse Practice Acts |
vocational nurse |
|
career ladder |
permissive licensure |
|
|
endorsement |
practical nurse |
Acronyms
|
AJN |
LVN |
|
ANA |
NAPNES |
|
ANCC |
NCLEX |
|
HOSA |
NFLPN |
|
ICN |
NLN |
|
LPN |
RN |
Nursing provides service to help people meet the daily needs of life when they have difficulty satisfying these needs on their own. As students, nurses bring certain knowledge, skills, attitudes, and abilities to their nursing program. They will develop skills and knowledge in school. Their ability to act independently will depend on their professional background, motivation, and work environment. Defining all the specific roles of a nurse is difficult because these roles constantly change. Factors that influence nursing activity include new discoveries in the biomedical field, development of new healthcare knowledge, changes in patterns of health services and payment, and the relationships among healthcare team members.
This topic discusses various programs for nursing education, approval and accreditation, licensure, the role and image of the nurse, and nursing organizations.
HEALTHCARE: A MULTIDISCIPLINARY APPROACH
The sophisticated healthcare system of the 21st century requires many trained individuals working together in a complex healthcare system (Box 2-1). Many contemporary healthcare positions originated as functions of either the physician or the nurse. For example, the duties of a hospital dietitian and the physical therapist started as functions of nursing. As knowledge of nursing and medicine grew, several segments of healthcare became their own professions. Healthcare has a tremendous variety of specialties and subspecialties. All healthcare positions have unique educational requirements.
BOX 2-1.
Allied Health Professionals
|
Chiropractor—Manipulates the musculoskeletal system and spine to relieve symptoms |
Paramedic—Trained in advanced rescue and emergency procedures |
|
Dental Hygienist—Trained and licensed to work with a dentist by providing preventive care |
Pharmacist—Prepares and dispenses medications by the primary care provider’s order |
|
Dietitian—Trained nutritionist who addresses dietary needs associated with illness |
Phlebotomist—Trained to perform venipunctures |
|
Electrocardiograph Technician—Assists with the performance of diagnostic procedures for cardiac electrical activity |
Physical Therapist—Plans and conducts rehabilitation procedures to relieve musculoskeletal disorders |
|
Electroencephalograph Technician—Assists with the diagnostic procedures for brain wave activity |
Physician’s Assistant (PA)—Trained academically and clinically to practice medicine under the supervision of a doctor of medicine or osteopathy |
|
Emergency Medical Technician—Trained in techniques of administering emergency care in route to trauma centers |
Psychologist—Trained in methods of psychological assessment and treatment |
|
Histologist—Studies cells and tissues for diagnosis |
Radiographer—Works with a radiologist or primary care provider to operate radiologic equipment for diagnosis and treatment |
|
Infection Control Officer—Identifies situations at risk for transmission of infection and implements preventive measures |
|
|
Respiratory Therapist—Trained to preserve or improve respiratory function |
|
|
Laboratory Technician—Trained in performance of laboratory diagnostic procedures |
|
|
Risk Manager—Identifies and corrects potential high-risk situations within the healthcare field |
|
|
Medical Assistant (Administrative or Clinical)—Assists the primary care provider in the front and/or back medical office, clinic, or other medical settings |
|
|
Social Worker—Trained to evaluate and correct social, emotional, and environmental problems associated with the medical profession |
|
|
Medical Secretary—Trained in secretarial sciences with an emphasis on medical applications |
|
|
Speech Therapist—Treats and prevents speech and language disorders |
|
|
Medical Transcriptionist—Trained in secretarial sciences to make typed records of dictated medical information Nuclear Medical Technician—Specializes in diagnostic procedures using nuclear devices |
|
|
Surgical Technician or Technologist—Assists primary care providers and nurses in the operating room |
|
|
Unit Clerk—Performs the administrative duties in a hospital patient care unit |
|
|
Occupational Therapist—Evaluates and plans programs to relieve disorders that interfere with activities |
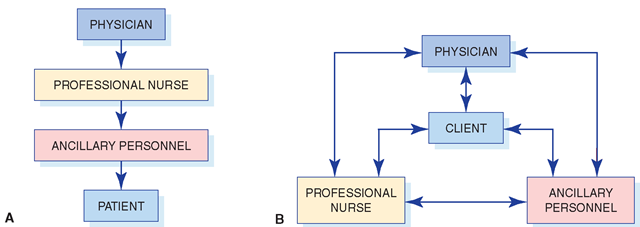
To achieve licensure as a physician, an individual starts with a minimum of 4 years of undergraduate study and continues with 4 years of medical school, after which the graduate doctor must take a licensure examination before practicing. As a new doctor of medicine, the physician who wishes to specialize must continue his or her education as a resident, which requires another 2 to 6 years of study. These years can be followed by additional years of advanced study. The physician is responsible for diagnosing and treating clients. In this role, the physician often acts as a team leader (Fig. 2-1).
TYPES OF NURSING PROGRAMS
Nurses are an important part of the healthcare team. Four basic types of educational programs lead to a credential in nursing (Table 2-1). Three programs allow the graduate to take the licensure examination and to become a registered nurse (RN). The fourth, a practical or vocational nursing program, allows the graduate to take the licensure examination and to become a licensed practical nurse (LPN) or a licensed vocational nurse (LVN). California and Texas use the term vocational nurse instead of practical nurse. This text utilizes three different but interchangeable abbreviations: LPN, LVN, and LPN/LVN.
FIGURE 2-1 · Traditional (A) and contemporary (B) views of healthcare practice.
TABLE 2-1. Nursing Practice and Educational Levels
|
CLASSIFICATION |
FUNCTIONS AND ROLE |
EDUCATIONAL REQUIREMENTS |
|
(Certified) Nurses Aide (CNA), Unlicensed Assistive Personnel (UAP) |
Provides basic nursing care for clients in a long-term care facility. Works under the supervision of an LVN, RN, or MD. In some facilities, the "aide” is referred to as Unlicensed Assistive Personnel. |
2 months to 6 months Educational requirements may differ between the CNA and the UAP. |
|
Licensed Practical/Vocational Nurse (LPN/LVN) |
Provides nursing care in long-term and acute care facilities. May also work in primary care providers’ offices and clinic settings. Works under the supervision of an RN or MD. |
1 to 2 years |
|
Registered Nurse (RN) |
Provides direct and indirect nursing care, supervision, and leadership in a wide variety of healthcare settings. |
2 to 4 years Associate’s degree (AD) or bachelor’s degree (BS or BA) or master’s degree (MS or MA) |
|
Advanced Practice Nurse or Nurse Practitioner (NP) |
An RN who receives additional training in a specialized field, such as pediatrics, maternity, geriatrics, family practice, or mental health. |
RN with a master’s degree plus additional and specific education and internship in the field of specialty |
Registered Nurses
Registered nurses spend from 2 to 4 years learning their profession. In addition, RNs may have special training that allows them to practice public health nursing or specialize in fields such as surgery. RNs are responsible for care of the acutely ill; teaching professional and practical nursing students; managing personnel; and taking charge in various healthcare settings. RNs also perform many duties that only physicians performed in the 20th century. For example, the RN may be first assistant in surgery. RNs may continue their education to become nurse anesthetists, nurse-midwives, or advanced practice nurses.
Basic Education
Three basic types of education lead to the RN license:
1. A student attends a 2-year program at a community or junior college and receives an associate’s degree (AD) in nursing. This AD-RN is educated primarily as a bedside nurse and is sometimes called a technical nurse. In some states, some nursing groups are advocating different licensure for RNs who graduate from AD programs, as opposed to graduates of 4-year programs.
2. The 3-year program was formerly sponsored by and based in a hospital. Most of today’s 3-year programs, however, are affiliated with community and state colleges that grant college credits. Some states no longer have 3-year programs.
3. The 4-year program in a college or university leads to a baccalaureate or bachelor’s degree in nursing. The graduate of this program may enter graduate school to study for an advanced master’s degree or doctorate. Most of these programs aim to prepare professional nurses who will be teachers or administrators or who will assume other leadership positions. Many bachelor’s degree graduates become certified as public health nurses and work in community health.
Some community colleges have programs that admit only LPNs, which, via a career ladder program, lead to an RN. The LPN is usually required to take general education courses before admission. Then, with approximately 1 additional year of education, an LPN becomes eligible to take the licensure examination and become an RN. This program leads to an associate’s degree.
Advanced Nursing Credentials
Several types of advanced certification are available to RNs. The American Nurses Credentialing Center (ANCC) of the American Nurses Association (ANA) grants a total of 27 advanced certificates.
Generalist nursing certificates require a bachelor’s degree and an examination. These certificates are available in 14 specialties including psychiatric-mental health, medical-surgical, gerontologic, perinatal, maternal-child, pediatrics, general practice, continuing education, and community health.
A clinical nurse specialist certificate is available in five areas of nursing: psychiatric-mental health-adult, psychiatric-mental health-child, medical-surgical, gerontologic, and community health.
An advanced practice nurse, formerly called the nurse practitioner, is an RN, usually with a master’s degree, who has specialized in a particular field. In addition to the RN license, the state issues a license to practice, or the state’s Nurse Practice Act grants authority to practice. The ANCC certifies advanced practice nurses in areas such as adult nursing, family practice, gerontology, pediatrics, and school nursing. Advanced practice nurses assess clients, assist in the diagnosis and treatment of illness, and, in many states, are authorized to prescribe medications. The roles of nurses with other additional educational preparation, such as midwives and anesthetists, are described later in this topic.
Practical Nurses/Vocational Nurses
Practical or vocational nurses are licensed under specific state laws (Nurse Practice Acts) to care for clients in various settings in the same manner as is the RN. Generally, the LPN/LVN works under the direct or indirect supervision of an RN or physician. The functions and responsibilities of the LPN/LVN and the RN often coincide. Many LPN/LVNs supervise nursing assistants or aides.
Do not confuse the position of the individual who is called a nurse’s aide, nursing assistant, certified nursing assistant (CNA), or unlicensed assistive personnel (UAP) with the LPN/LVN or RN. Although the aide may receive a certification by the state when completing a nurse aide training course, this individual is not licensed, and therefore not regulated by a state nurse practice act. A nursing assistant, aide, or UAP is a person who is taught via on-the-job training or in short-term programs to help clients and residents meet the needs of daily living, such as hygiene and dressing.
Current functions of the LPN/LVN include providing bedside care, doing wound care, administering prescribed medications, monitoring client status, and reporting reactions to medications or treatments to the RN or physician. Individual states or healthcare agencies may limit the LPN/LVN’s care of intravenous lines, complex treatment and medication regimens, and functions related to primary or complex healthcare assessment of clients.
Standards of nursing practice of LPN/LVNs are promoted by the National Association for Practical Nurse Education and Service, an association for the representation of LPN/LVNs. Another association, the National Federation of Licensed Practical Nurses, also promotes standards of practice for the practical/vocational nurse. These two major nursing organizations are discussed later in this topic.
According to the Bureau of Labor Statistics Occupational Outlook Handbook for December 2008, most practical/ vocational nurses work in acute care hospitals, long-term care facilities, physician offices/clinics, home healthcare services, outpatient care centers, and government agencies (e.g., correctional facilities or military reserve). Growth in employment opportunities for the LPN/LVN is projected to be in long-term care facilities and home healthcare services.
Practical/Vocational Nursing Education
Most practical/vocational nursing programs exist under the auspices of a high school, a vocational institute, a proprietary college, or a community college. Such diverse institutions as hospitals and universities administer some programs. The number of state-approved practical/vocational nursing programs has grown to include nearly 2,000 programs in the United States. Canada also has a number of programs. Further data can be found through the United States Department of Labor website (refer to Web Resources on Point-’-). The growth of LPN/LVN programs is an indicator of the need for nurses, both LPN/LVNs and RNs. Because they depend on the availability of clinical sites, RN programs can only accept a certain number of students. In the 1990s, some RN programs closed, as they were not cost-effective for the college or university. (Some of these have reopened due to the nursing shortage and the federal and state availability of funds for nursing students and nursing programs.) Also, there is currently a great shortage of nursing instructors in both LVN and RN programs. Thus, an alternate route to the RN licensure is via a LPN/LVN to RN career ladder. This approach has the dual benefit of allowing graduate LPN/LVNs to work as licensed nurses while attending RN programs.
Curricula are designed to include classroom theory in the various aspects of nursing. The student then has an opportunity to practice clinical skills in a hospital, nursing home, community health agency, or other health-related facility. Classroom theory and clinical practice are correlated as closely as possible to ensure maximum retention of skills. Most practical nursing programs are the equivalent of 12 to 18 months of full-time study. Many LPN/LVN to RN Career Ladder programs generally accept the LPN/LVN curricula in place of the first year of RN curricula, which often means that the LPN/LVN may not need to take the fundamental and/or beginning level RN courses of an RN program. Both LPN/LVN and RN programs require additional general education or specific science-related classes that enhance the content of nursing courses. Each school will have educational counselors or advisors who will be able to provide unique advice to each student in his or her choice of general educational or nursing-related courses.