Prevention of Later Postoperative Complications
Dangers of prolonged bed rest following surgery include respiratory and circulatory complications, including hypostatic pneumonia, blood clots (thrombophlebitis or DVT—deep vein thrombosis), pulmonary embolism, development of pressure ulcers, generalized edema, contractures, difficulty in weight-bearing and balance, formation of renal calculi, scrotal edema, constipation, urinary retention, loss of appetite, and general depression and disorientation. Consequently, the sooner the client can move about after surgery, the better it is for the client.
Key Concept Postoperative skin assessment is particularly important, as the client may have remained in the same position for an extended period of time in the OR and PACU.
Postoperative Activity. Follow the instructions of the primary provider. At first, the client may dangle his or her legs over the edge of the bed, then sit in a chair, and finally walk.The nurse helps clients to ambulate as soon as possible after surgical procedures, according to the surgeon’s orders. Early ambulation, preferably on the day of surgery, assists circulation, improves respiration, prevents lung congestion, and aids in voiding and bowel activity. The client who is out of bed and walking will eat better and sleep more soundly. He or she can become more self-sufficient, promoting a rapid recovery. Many subsequent disorders are prevented by early ambulation.
Respiratory Complications
A high percentage of complications following surgery are respiratory in nature. Respiratory insufficiency (hypoventilation) leads to hypoxemia, and may cause respiratory arrest. Other respiratory complications include hypostatic or aspiration pneumonia (inflammation of the lung or accumulation of fluid in the lung) and atelectasis.
Aspiration pneumonia can result when fluid or mucus is aspirated or sucked into the lungs. Inhibition of normal clearance mechanisms (e.g., coughing) caused by anesthesia can lead to aspiration pneumonia. Hypostatic pneumonia is caused by immobility, particularly lying on the back. This condition does not involve invasion by microorganisms. Postoperative pneumonia caused by infectious microorganisms is less common.
Atelectasis is the collapse of air sacs in the lungs, usually caused by mucous plugs that close the bronchi and may involve all or part of a lung. The postoperative client often is reluctant to cough or breathe deeply because of incisional pain: this can lead to atelectasis. This client may become somewhat cyanotic as respirations and pulse become very rapid and breathing becomes difficult.
An important nursing responsibility is preventing postoperative respiratory complications. Listen to lung sounds at least once per shift for evidence of fluid accumulation, dyspnea, atelectasis, or other respiratory symptoms.Other important signs are fever and cyanosis.
Prevention of Respiratory Complications. Respiratory exercises or treatments (e.g., turning, coughing, and deep breathing; TCDB), chest percussion, and using the incentive spirometer can reduce or eliminate respiratory complications (see In Practice: Nursing Care Guidelines 56-3). Be sure to encourage ambulation as well.
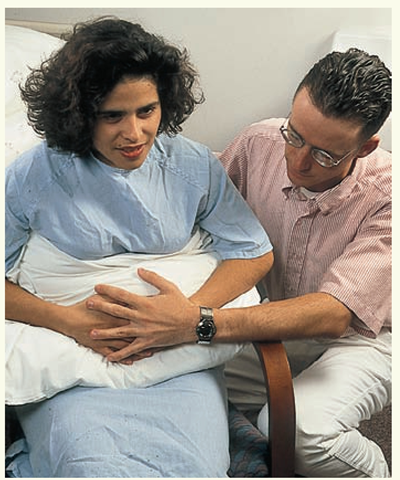
Splinting the incision helps relieve some pain and discomfort the client may experience during coughing (see Fig. 56-3B). Be sure to provide ample analgesia about one half hour prior to coughing and deep-breathing exercises. Rationale: This helps to maximize pain relief.
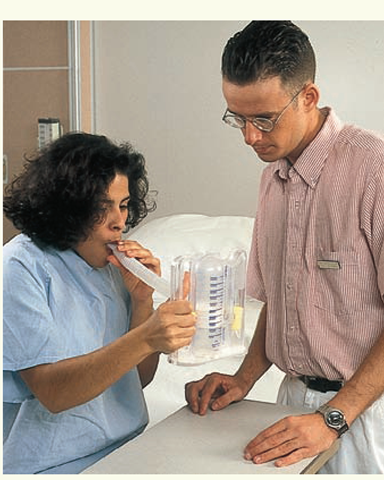
The incentive spirometer, which forces the client to concentrate on inspirations while providing immediate feedback, aids deep breathing (see Fig. 56-4). Incentive spirometers come in two types: flow activated and volume activated. The flow-activated incentive spirometer usually consists of one or more balls in a vertical tube. Because deep breaths (volume) are the objective, the length of time the client suspends the ball at the top of the tube determines the depth of the breath. Volume-activated devices come in many shapes, but because they measure volume directly, they make it easier for the client to understand when he or she has accomplished a deep breath.
Key Concept Breathing exercises will be more effective if the client learns and practices them preopera-tively The client takes the incentive spirometer home at discharge, so these exercises can be continued.
Circulatory Complications
Serious circulatory complications can develop postoperatively.
Thrombophlebitis and Deep Vein Thrombosis. A dangerous circulatory complication is thrombophlebitis, the inflammation of a vein associated with formation of a blood clot, a thrombus. This condition is known as deep vein thrombosis (DVT). It is caused by venous stasis (the slowing or stopping of venous blood return) as a result of increased clotting, lack of activity, increased pressure within vessels, and other factors. It most often develops in the calves of the legs. Clients at highest risk for DVT are those over age 40 with prior thromboembolism and who are undergoing major surgery on the lower extremities. This particularly includes those who are having hip or knee replacements. Other risk factors include obesity, smoking, and a sedentary life style. These clients are often given preoperative prophylactic medications. In addition, the use of graduated compression stockings and intermittent pneumatic compression devices can help prevent DVT.
IN PRACTICE: NURSING CARE GUIDELINES 56-3
ASSISTING THE CLIENT WITH POSTOPERATIVE EXERCISES
General Guidelines
♦ Remember that the postoperative client will be better able to perform these exercises if he or she learns them during the preoperative period.
♦ Wear gloves for these procedures if the client has any open drainage.
♦ Explain procedures to the client before you assist with them.
♦ Document all procedures and results.
Splinting an Incision
♦ Splinting relieves pressure on the abdominal suture line and thus relieves pain.
♦ Use a pillow, folded bath blanket, or large towel as a splint to distribute pressure evenly across an incision. Assist the client to hold the splint for the first few days after surgery, The client will be able to hold it in place after that.
♦ Grasp the pillow or bath blanket at the edges and stretch it across the client’s incision. Hold it from behind or press firmly on the front.
Holding a pillow or a folded bath blanket and pulling it tightly against the incision splints the incisional area. This technique helps to make coughing or deep breathing more comfortable and promotes better oxygenation.
♦ Apply pressure firmly by pushing down on the splint for the client who is lying in bed, or by pulling the splint toward you from behind when the client is sitting. Do this as the client coughs.
♦ Anticipate the timing and strength of each client’s cough. Count aloud and feel the movement of the client’s breathing as he or she prepares to cough.
Turning, Coughing, and Deep Breathing (TCDB)
♦ Instruct the client to take a deep breath and hold it for 2 to 5 seconds. Rationale: Holding a deep breath allows air to reach the lung’s most severely deflated areas.
♦ Instruct the client to do a strong double-cough with the mouth open. Rationale: The double-cough maneuver helps the client to mobilize and remove secretions.
Instruct the client to take a deep breath, hold it for 2 to 5 seconds, and then do a strong double-cough (or “hack out” three short coughs) with the mouth open.
♦ Repeat this process several times each hour, especially for the first few days after surgery and while the client remains bedridden.
Huffing
♦ Teach the client to take a deep abdominal breath and then force air out in several short, quick breaths. The client should then take a second, deeper breath and force it out in short, panting movements. The client should then take an even deeper third breath and exhale it quickly in a strong huff. Rationale:This series helps to loosen more secretions than just coughing.
♦ Instruct the client to repeat this series of breaths as many times or for as long as is ordered.
Using the Incentive Spirometer
♦ Position the client as upright as possible without causing discomfort. Rationale: An upright position allows the client to maximize the use of his or her diaphragm.
♦ Explain the operation of the spirometer to the client. Set a goal, number of seconds, or specific volume to be attained. Agree on the number of times and how often the procedure is to be done, within physician’s orders.
♦ Instruct the client to cough to remove as much mucus as possible before the treatment. Rationale:This action enables the client to achieve the maximum inhalation.
♦ Teach the client to take slow, deep breaths and to hold each breath at the end of inspiration for 2 to 5 seconds. Rationale: Doing so allows air to reach the lung’s most severely deflated areas.
♦ Repeat the procedure until the client has achieved the established goal or has given his or her best effort at least 8 to 10 times. Ensure that the client does not repeat the process too rapidly Rationale: You do not want the client to inadvertently hyperventilate.
♦ Instruct the client to repeat coughing or huffing at the procedure’s end. Rationale:The client must clear his or her lungs as much as possible.
NURSING CARE GUIDELINES 56-3 continued
Using the spirometer. The client can observe her progress by watching the diaphragm rise in the tube. This exercise should be repeated 5 to 10 times every hour.
• Dispose of gloves and wash hands thoroughly at the end of the procedure. Rationale:These procedures reduce the risk of infection transmission.
Leg Exercises
• Position the client in a semi-Fowler’s position.
• Have the client wiggle the toes. Rationale: This is the first action that the client can do immediately after surgery. This activity helps to promote circulatory function.
• Bend the client’s knee and raise his or her foot. Hold this position for a few seconds.
• Extend the client’s leg and lower it to the bed.
• Do this five times for each leg. Rationale: Repetition helps to maintain muscle tone and decrease venous stasis.
• Have the client trace circles with the feet by bending them down, in toward each other, up, and then out. Repeat this procedure five times with each foot. Rationale: This motion promotes circulation and contributes to optimal respiratory exchange.
• Position the client in a side-lying position.
• Flex and extend the client’s hip joint by using a bicycling motion. Repeat this five times on each side. Rationale: This motion promotes contraction of the muscle, which is strengthened with repetition.
• Encourage the client to exercise his or her legs as much as possible when in bed. Rationale: These actions promote circulatory function and prevent contractures, foot drop, and other complications.
Symptoms of DVT and thrombophlebitis include swelling, warmth, redness, and tenderness in the area. To test for thrombophlebitis, flex the client’s foot up toward the knee (dorsi-flexion) with the leg straight. If pain occurs behind the knee on dorsiflexion, it is known as a positive Homans’ sign, indicating probable thrombophlebitis. Instruct the client to remain in bed, and report this finding immediately.
If thrombophlebitis occurs, the following supportive measures may be ordered by the primary healthcare provider:
• Elevate the affected body part on a soft pillow when in bed.
• Administer thrombolytics and/or anticoagulants, as directed (see below)
• Avoid rubbing the body part (may dislodge clot).
• Apply warmth as directed .
• In rare cases, maintain the client on strict bed rest.
Embolism. An embolus (plural, emboli) is a piece of a clot or thrombus that breaks off and enters the person’s circulatory system, usually obstructing the blood flow in a smaller vessel (embolism). Symptoms of embolism depend on its location, but include severe pain and shock, and may include nausea and vomiting, as well as other symptoms. Probably the most life-threatening embolism is a blood clot that lodges in the small vessels of the lung, a pulmonary embolism. Signs of a pulmonary embolism include difficult breathing, sharp chest pain, cough, cyanosis, rapid respirations and heart rate, and severe anxiety (Taylor, Lillis, LeMone, & Lynn, 2011). A pulmonary embolism rapidly can be fatal.
If the embolism is in an arm or leg, circulation distal to the embolus is often cut off, causing related symptoms, such as numbness, pain, and absence of pulse. An embolism often can be treated with the immediate administration of special medications that dissolve or split up existing blood clots (thrombolytic agents). Examples include alteplase, recombinant (Activase), a thrombolytic enzyme, and the thrombolytic agent, streptokinase (Streptase). These agents must be used with caution after surgery because they may interfere with clot formation in the surgical incision, while dissolving the thrombi that caused the embolism. These medications are also used cautiously in clients with liver disorders.
One means of avoiding circulatory disorders is to apply elastic stockings, elastic roller bandages, or antiembolism (TED) stockings as ordered by the primary healthcare provider. Other nursing measures used to prevent circulatory disorders include performing leg exercises every 2 hours, complete range-of-motion exercises every shift, and ambulation as soon as possible after surgery. In some cases, a pneumatic/sequential compression device is used. This device helps to keep blood circulating by alternating external pressure on the legs.