Physical Examination and Laboratory Tests
Before surgery, the client undergoes a complete physical examination, including laboratory tests. This is done about a week before the procedure in nonemergency surgery. Routine, preoperative tests often include a chest x-ray, complete blood count (CBC), and urinalysis (UA). A metabolic panel is often done, as well as a toxicology screen, if there is a possibility of alcohol or drug abuse. A pregnancy test may be done, to determine what, if any, medication can be used. Other tests and examinations are performed as needed. An electrocardiogram is usually obtained for all clients older than 40 years. Blood is drawn for a type and cross match if any possibility exists that a blood transfusion will be needed during surgery. In this case, two blood ID bands must be worn, in addition to regular ID bands. A bleeding-clotting test, such as the prothrombin time, is often ordered.
Vital signs recorded during the physical examination are used as baseline data for comparison during and immediately after surgery. The client’s weight is documented in the health record in kilograms, because dosages of medications, including anesthetics, are usually calculated on the basis of the client’s kilogram weight.
Key Concept The physical examination, laboratory tests, and other tests are all done before the client comes to the facility for surgery unless the surgery is an emergency.
Notify the physician of routine medications the client takes. Information about allergies and the wearing of an allergy ID band are necessary for all clients. If the client has no allergies, an allergy band stating this fact is worn. An allergy to latex is particularly important because some materials used in surgery and after surgery (e.g., catheters, chest tubes, gastric drains) are latex, unless a substitute is required. See the Nursing Process display at the end of this section.
Skin Preparation
If an incision is to be made in the skin, skin preparation is necessary. The skin, which is normally oily, harbors bacteria and must be thoroughly cleansed before surgery to help prevent wound contamination and subsequent infection. Usually, the client is required to shower with antibacterial soap at home or in the hospital several hours before surgery. The operative site is further prepared just before or after the client is anesthetized. The skin is cleaned with an anti-infective agent and may be shaved, because microorganisms adhere to hair. These procedures are known as a surgical preparation or “prep.” Most often, the prep and shave are performed in the OR to further reduce the risk of infection. If the nurse is expected to perform this procedure, specific instructions will be needed.
Intestinal Preparation
The surgery, the anesthetic, and the client’s condition determine if intestinal preparation is needed and, if so, what type. In many surgical procedures and examinations, such as colonoscopy, the intestinal tract should be as empty of feces as possible. If surgery is in the abdomen or pelvis, and in some other cases, the client will likely receive one or more enemas to empty the bowel.Be sure the client expels the entire enema because an anesthetized client may expel the remainder on the operating table, contaminating the operative site. Enemas are often done at home. A self-contained enema, such as the Fleet, is easy for the client to self-administer.
A client also may be required to drink a cathartic solution to cleanse the bowel. In some cases, the client must take a large amount, as much as several quarts, of solution such as polyethylene glycol-electrolyte solution (GoLYTELY) or another bowel preparation called Halflytely. The client needs encouragement and positive reinforcement to complete this task. Alternatives, such as magnesium citrate or MiraLax, are presently frequently used.
If the client is to have spinal or general anesthesia or conscious sedation, he or she is asked to remain NPO (nothing by mouth) for at least 8 to 10 hours before surgery to minimize the possibility of nausea and vomiting during anesthesia. In some cases involving extensive local anesthesia, or if there is any chance of an emergency requiring general anesthesia, maintaining NPO status is also needed. If vomiting does occur, aspiration is less likely if the client’s stomach is empty.
Key Concept The client may be asked to self-administer a small-volume enema or drink a liquid cathartic at home if the admission to the healthcare facility is on the day of surgery The client may need instruction in the use of the enema or the cathartic. Encourage the client and reassure that he or she will be able to do the procedure. Be sure the client has an escort if same-day surgery is being done.
Preoperative Medications
Four types of medications commonly are used preopera-tively: sedatives, antibiotics, narcotics, and drying agents.
Because the client should have as much rest as possible before surgery, a sedative is usually ordered the evening before surgery so that the client can sleep. This is a one-time only order. Sedation also helps to stabilize BP and pulse.
Most surgeons prescribe antibiotics before surgery to help prevent postoperative infections. These are usually taken for several days before surgery.
On the morning of surgery, a preoperative narcotic is given to relax the client and enhance the anesthesia’s effects. It may be ordered for a specific time of day or “on call to OR.” In the latter case, the medication is taken when the OR is ready for the client.
A drying agent/anticholinergic, such as atropine sulfate (AtroPen, Sal-Tropine), is given to help inhibit body secretions so the client produces less mucus, reducing the likelihood of aspiration and atelectasis (collapse of the tiny air sacs in the lungs). Production of gastric and intestinal secretions is also reduced, so there is less abdominal distention postoperatively. Atropine may contribute to postoperative constipation and other gastrointestinal (GI) complications.
Key Concept Before giving any preoperative medications, make sure the client does not have any drug allergies and that the surgical permit has been signed, witnessed, and is on the client’s chart or electronic record. Make sure the client is wearing an allergy band, whether or not an allergy exists. The client may be given regular medications, such as those for HTN, before surgery
Before giving preoperative medications, ask the client to go to the bathroom. Explain to the client the purpose of any drug and its probable effects. Ask again about any drug allergies before giving medications. Explain to the client that after the narcotic or other presedation medication has been given, the side rails will be raised, that he or she must remain in bed, and that he or she should request assistance to go to the bathroom. Explain to family members that the client has received sedative medication and that, although they may sometimes stay in the room, they should allow the client to rest and not carry on a conversation. In Practice: Important Medications 56-1 provides additional information.
Key Concept Be sure to offer a bedpan or urinal to the client immediately before he or she is taken to the OR. The client should not get up to the bathroom at that time.
Client Transport
If the client is in the hospital preoperatively, prepare the client’s room. (This procedure is described later in this topic.) Make the client as comfortable as possible. Make sure the preoperative checklist in the client’s health record is complete and signed; the record will accompany the client to the OR or it will be entered into the computer where it will be available to the anesthesia personnel or the OR nurse. Note on the front of the record if the client has any drug allergies or is taking cortisone, insulin, blood pressure medication, an anticonvulsant, or an anticoagulant. In some facilities, ID bands will identify these medications as well. Make sure the client is wearing all the appropriate ID bands. Send a clean bath blanket with the client.
Nursing Alert To prevent errors, always be certain the client is properly identified before transfer to the OR. No client is allowed to go to the OR without an identification bracelet! This would cause the surgery to be cancelled. Some hospitals require an ID bracelet on both of the client’s wrists. The client also must be wearing an allergy band, stating existing allergies or stating that the client has no known allergies. If the client is a fall risk, a fall risk ID band is worn as well. A client over age 65 is usually automatically considered to be a fall risk. Two blood ID bands also must be worn if the client will receive blood transfusions. The ID bands of the client going to surgery must be checked by at least two staff people and verified by the client/family before the client enters the OR.The client/family also must verify the type of surgery to be done.
NURSING PROCESS
ASSESSMENT AND DATA GATHERING PRIORITIES
• Nursing history
• Client’s understanding of the proposed surgical procedure (clarify any misperceptions)
• Past experiences with surgery
• Fears (fear of the unknown, fear of pain or death, fear of changes in body image or self-concept)
• Factors that increase surgical risk or the potential for postoperative complications:
• Past and present illnesses: Cardiovascular diseases, pulmonary disorders, alterations in renal and liver function, metabolic disorders (especially diabetes)
• Medications: Such as anticoagulants, diuretics, tranquilizers, adrenal steroids, antibiotics
• Lifestyle factors: Nutrition (history of eating disorders, malnutrition, or obesity); use of alcohol, nicotine, or recreational drugs; activity level; use of herbal supplements (many are mild anticoagulants or can adversely interact with medications)
IN PRACTICE: IMPORTANT MEDICATIONS 56-1
EXAMPLES OF IMPORTANT PREOPERATIVE AND INTRAOPERATIVE MEDICATIONS
Sedatives Used as Premedication Before Anesthesia
♦ pentobarbital Na+ (Nembutal)—especially in pediatrics
♦ phenobarbital Na+ (Luminal)—oral or parenteral
♦ promethazine (Phenergan)—used pre- or postoperatively, and in obstetrics
♦ midazolam HCl (Versed)—benzodiazepine, central nervous system [CNS] depressant, anxiolytic; causes some amnesia, can be used alone for conscious sedation
Sedatives Used to Assist Clients to Sleep
♦ chlorpromazine (used in Canada)—especially to relieve preoperative apprehension, also antiemetic
♦ estazolam (ProSom)
♦ flurazepam HCl (used in Canada)
♦ temazepam (Restoril)—used pre- or postoperatively
♦ secobarbital Na+ (Seconal Na+)—also can be premedication
♦ zolpidem (Ambien)—used pre- or postoperatively
Antibiotics and Cephalosporins
♦ amoxicillin trihydrate (Amoxicillin)
♦ ampicillin—used in some high-risk clients undergoing cesarean section
♦ cefotaxime Na+ (Claforan)
♦ ceftriaxone Na+ (Rocephin)—used especially in coronary surgery and in potentially contaminated procedures
♦ cefoxitin sodium (Mefoxin)
♦ cefuroxime axetil (Ceftin)
♦ ertapenem (Invanz)—used in adults to prevent infection after colorectal surgery
♦ erythromycin—used in clients allergic to penicillin, with valvular heart disease
♦ metronidazole (Flagyl)—used especially in colorectal surgery
♦ penicillin (various forms)
♦ vancomycin HCl (Vancocin)—used in clients allergic to penicillin
Narcotics
♦ fentanyl (Sublimaze)
♦ meperidine HCl (Demerol HCl)
♦ morphine SO4 (Morphine)
Drying Agent
♦ atropine sulfate (anticholinergic)—prevents or reduces respiratory tract secretions
Nursing Considerations
When Sedatives and Narcotics are Given
♦ Observe for respiratory distress or bradypnea (very slow respirations). These medications often are contraindicated in clients with severe respiratory disorders.
♦ Observe for inability to arouse client, extreme lethargy or drowsiness, fatigue, or oversedation.
♦ Observe for other CNS symptoms, such as dizziness, blurred vision, severe nightmares, ataxia (difficulty in coordination).
♦ Keep in mind that the medications may potentiate (abnormally enhance) the action of oral anticoagulants and antihypertensive drugs.
♦ Watch for paradoxical excitement in older adults or children (a reaction opposite the desired reaction).
When Antibiotics are Given
♦ Instruct the client to inform the caregiver of any untoward effects, such as a rash, stomach upset, or diarrhea.
♦ Instruct the client to drink plenty of water
♦ Some antibiotics are to be taken on an empty stomach and some with food. Check the specific instructions.
♦ Instruct the client to take all of the medication for the prescribed length of time.
♦ If the client is taking an oral contraceptive, advise her to use another means of fertility control while taking antibiotics.
♦ Avoid alcohol.
When Atropine is Given
♦ Know that atropine is given cautiously to clients with glaucoma and certain other eye disorders and may be contraindicated. Atropine is also contraindicated in clients with certain gastrointestinal (GI) conditions, such as achalasia, peptic ulcer, or pyloric obstruction, and with asthma, chronic obstructive pulmonary disease (COPD), heart conditions, symptomatic prostatic enlargement, Down syndrome, brain damage, and liver or kidney dysfunction.
♦ Inform the client about the experience of a dry mouth; relieve with moistened cloth, ice chips, sips of water and hard candy as tolerated and allowed. Report if dry mouth does not gradually resolve postoperatively.
♦ Observe for side effects such as dizziness, agitation, confusion, diarrhea, constipation, urinary retention, blurred vision, and sensitivity to light.
♦ Be alert for other more serious side effects, including skin rash, eye pain, difficulty breathing, irregular heartbeat, hallucinations, and difficulty swallowing. Report any of these immediately.
• Adequacy of coping patterns and support systems
• Pertinent sociocultural factors (e.g., health beliefs and practices, economic concerns, cultural considerations such as language barrier problems and ethnic beliefs related to surgery and healing)
• Vital signs the morning of surgery (report any significant deviation from normal)
• Accurate height and weight (medications may be calculated on the basis of these data, especially for children)
• General systems review, noting in particular any new cardiopulmonary developments that place the client at high risk during surgery
• Results of all preoperative diagnostic tests recorded in the client’s record and, if abnormal, reported to the surgeon or their representative
• Presence of an escort or driver (for transportation home with same-day surgery)
POSSIBLE NURSING DIAGNOSES
• Anxiety
• Ineffective Coping
• Decisional Conflict
• Fear
• Anticipatory Grieving
• Deficient Knowledge
• Powerlessness
PLANNING
Design a plan of care with the client and family to achieve the following general client goals. Before surgery, the client:
• Demonstrates physical preparedness for surgery (absence of significant deviations from normal in vital signs; no signs of infection)
• Verbalizes any concerns or fears related to the surgery
• Provides informed consent for the surgery
• Correctly demonstrates how to turn, deep breathe, use equipment (e.g., the incentive spirometer), and perform splinting of incision, when appropriate
• Correctly demonstrates how to use any special equipment that will be in place following surgery
• Verbalizes understanding of postoperative pain management program
• Verbalizes understanding of postoperative activity plan
• Demonstrates the presence of adequate caregivers at home after discharge
IMPLEMENTATION
• Establish a supportive and trusting nurse-client relationship.
• Develop and implement a teaching plan that:
• Familiarizes the client and family with what to expect on the day of surgery
• Prepares the client to participate in the pain management program
• Enables the client to state the purpose of deep breathing and to demonstrate it, as well as procedures such as incentive spirometry, leg exercises, and turning in bed
• Counsel the client and family about helpful coping strategies and available resources. At the client’s request, invite a spiritual counselor to see the client.
• Maintain nutrition and hydration; if the client is to be NPO (nothing by mouth) for 8 to 12 hours before surgery, ensure that the client understands the reason for this restriction, and remove all food and fluids from the bedside. If the client is in the facility, place an NPO sign on the door of the room. If the client performs preparation at home, make sure that he or she remained NPO.
• Evaluate the client’s bowel status and determine the need for an order for bowel elimination.
• If an indwelling catheter is ordered before surgery, explain its use before insertion.
• Carry out preoperative skin and hygiene orders.
• Facilitate sleep and rest in the immediate preoperative period. A sleeping aid may be ordered.
• Remember that many clients are not admitted until the morning of surgery. The nurse must determine what teaching has been done previously and perform the remainder of the preoperative teaching at that time.
EVALUATION
Determine the adequacy of the plan of care by evaluating the client’s achievement of the preceding identified preoperative goals. If the client is unable to meet key goals, modify the plan. Key evaluative criteria:
• Client’s physical preparedness for surgery
• Client’s mental preparedness for surgery
• Client’s understanding of, and ability to, participate in care postoperatively
• An uneventful course of recovery
The client’s family is included in all preparation as needed.
INTRAOPERATIVE NURSING CARE
Observing a client undergoing surgery may be a component of a nursing student’s experience. If this is possible, take advantage of the opportunity. Doing so will give you a better idea of surgical procedures and the atmosphere of the operating room. Many graduate nurses are specially trained to work in the OR or PACU.
Key Concept Observing surgical procedures aids in understanding the clients feelings and apprehensions and why a postoperative client experiences pain and discomfort.
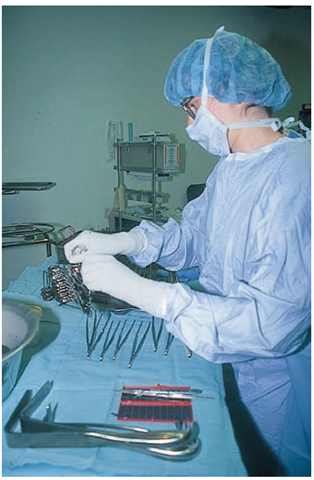
Nurses and surgical technicians assist surgeons in the operating room. The categories of staff working with the surgeon include the sterile assistant(s) (scrub assistant) and the circulating nurse(s). The sterile assistant, an RN, specially trained licensed practical nurse or licensed vocational nurse (LPN/LVN), or OR technician, is scrubbed, gowned, and gloved. He or she functions within the sterile field. Duties include positioning and draping the client, handing instruments and medications to the surgeon, threading needles, cutting sutures, assisting with retraction and suction, and handling specimens (Fig. 56-5).
FIGURE 56-5 • The scrub nurse or technician prepares sterile instruments for the surgeon’s use.
Another person who may work in the OR is the registered nurse first assistant (RNFA). This person functions under the supervision of the surgeon and performs more complex duties than the sterile scrub assistant. For example, the RNFA may assist with suturing the incision or by providing hemostasis (stoppage of bleeding).
The circulating nurse (circulator) is an RN who works in the OR, but outside the sterile field. Duties include general management of the operating suite, including monitoring temperature, cleanliness, humidity, lighting, and fire safety. This nurse continually assists the anesthesia personnel in monitoring the condition of the client and observes for breaks in technique by ancillary personnel entering the area, such as laboratory or x-ray personnel. The circulator also assists by opening sterile packs, delivering sterile supplies and instruments to the sterile team, delivering medications to the scrub person, weighing and labeling specimens, and keeping records during the surgical procedure.