Abstract
The autonomic nervous system (ANS) plays an important role in the pathophysiology of arrhythmogenesis due to increased sympathetic activity and reduced vagal tone. Traditional time and frequency heart rate variability (HRV) parameters have gained importance in recent years as techniques employed to explore the ANS. Available data support conclusions that decreased HRV is a strong predictor of increased cardiac mortality. On the other hand, inteventions that tend to increase HRV, such as regular sports activity, may have a cardio-protective effect. However, when analysing the effects of different sports disciplines and the effects of strenuous exercise on the cardiac autonomic function determined by HRV indices results remain conflicting due to a variable behavior of the used HRV time domain and spectral parameters.
Introduction
In the course of the last two decades numerous studies in both animals and human beings have shown a significant relationship between the ANS and cardiovascular mortality. Perturbations of the ANS and its imbalance consisting of either increased sympathetic or reduced vagal activity may result in ventricular tachyarrhythmias and sudden cardiac death, which is presently one of the leading causes of cardiovascular mortality. [1] Conversely, increased vagal tone associated to decreased sympathetic activity may improve the cardiovascular status. In this context, one of the most efficient means to reach this improvement is to perform regular physical activity.
This article reviews the structure and function of the ANS, its relationship with the normal and diseased heart, and the effects of regular sports activity and of strenuous exercise on the ANS using HRV to explore it.
Structure and Function of the Autonomic Nervous System
The ANS is composed of elements arising from the central and peripheral nervous systems and regulates the activities of structures not normally under voluntary control.[2, 3] It is predominantly an efferent system composed of the sympathetic and parasympathetic branches transmitting impulses from the central nervous system to the periphery (heart, arteries, veins, lungs, etc). While the sympathetic fibers are widely distributed throughout the body, the parasympathetic fibers supply more specific structures. These two divisions of the ANS are in many instances in functional opposition, but in other instances are synergistic. Their most important role is to preserve the body’s ability to maintain internal stability or equilibrium and to balance opposing actions under the control of higher cerebral centers. [2, 3] In contrast to the parasympathetic system, the sympathetic system enables the body to respond to challenges to survival (fight or flight) or situations of hemodynamic collapse or respiratory failure. Sympathetic responses include an increase in heart rate (HR), blood pressure, and cardiac output; a diversion of blood flow from the skin and splanchnic vessels to those supplying skeletal muscle; bronchiolar dilation and a decline in metabolic activity.
The Autonomic Nervous System and the Normal Heart
The electrical and contractile activity of the myocardium is constantly dependent on the ANS. In physiological conditions, the sympathetic and parasympathetic branches have opposing actions on the different cardiac functions. The role of the ANS is to adapt the functions of the cardiac pump to the potential requirements of the body. [2, 3] The ANS regulates HR, myocardial contractility and vascular peripheral resistance, thereby controlling blood pressure, cardiac output and overall stability of the cardiovascular system. Neurohumoral regulation can produce important and rapid cardio-circulatory changes in a few seconds before other much slower mechanisms, such as those mediated by metabolic stimuli, circulating catecholamines or the renin-angiotensin system, exert any effect. [4]
Effects of Autonomic Nervous Regulation on the Heart
Although cardiac automaticity is intrinsic to different tissues with pacemaker properties, HR and cardiac rhythm are under the influence of the ANS. [5-7] Both divisions of the ANS tonically influence the cardiac sinus node. The sympathetic system enhances automaticity, whereas the parasympathetic system inhibits it.
Modulation of cardiac automaticity depends on intra-sinus displacements of rhythm control at the tissue level and on changes of ionic currents at the cellular level. Three types of ionic current are implicated in the regulation of slow diastolic depolarization of the pacemaker cells and are modulated by the ANS: the potassium current IKAch, the calcium current ICa and the hyperpolarization-activated "pacemaker" If current.
Interaction of Sympathetic and Parasympathetic Effects
Vagal and sympathetic activity constantly interact. However, under resting conditions in a normal subject, vagal tone predominates and variations in HR depend mainly on vagal modulation. Vagal tone has an inhibitory effect on sympathetic activity because of the presence of acetylcholine which attenuates adrenergic stimulation and diminishes release of norepinephrine. Sympathetic activation becomes significant at a low effort level or under any external influence. Administration of atropine results in immediate tachycardia while B-adrenergic blockade only induces a weak decrease in HR at rest.
The Autonomic Nervous System and Heart Diseases
The ANS intervenes not only in various normal situations, but also in pathological situations, and thus may induce deleterious effects on the heart. Abnormalities of the ANS have been demonstrated in diverse conditions such as diabetic neuropathy, [8] coronary heart disease, particularly in the context of a myocardial infarction, [9] and in congestive heart disease. [10]
It is clearly established nowadays that a dysregulation in the autonomic nervous control of the cardiovascular system associating increased sympathetic and reduced parasympathetic tone plays an important role in coronary artery disease and in the genesis of.life-threatening ventricular arrhythmias. Increased adrenergic tone probably initially induces a dysfunction at the level of the vascular endothelium, which serves a dual role in the control of vascular tone by secreting both vasorelaxing (nitric oxide and prostacyclin) and vasoconstricting factors (endothelin-1). [11] Increased adrenergic tone may subsequently damage the endothelial bareer resulting in release of vasoactive substances, platelet aggregation and initiating thereby a mechanism for the formation of an atherosclerotic plaque and the risk of developping ischemic heart disease. [11]
The occurrence of ischemia and/or myocardial necrosis may induce a mechanical distortion of the afferent and efferent fibers of the ANS due to changes in the geometry related to necrotic and noncontracting segments of the heart. These geometrical ischemic changes result in denervation of myocardial regions, rendering the myocardium more sensitive to catecholamines. [12] Moreover, the resulting sympathetic overactivity may further increase platelet activation and coronary vasoconstriction, and be responsible for the development of ventricular arrhythmias. Available experimental and clinical data suggest that sympathetic overdrive may favor the incidence of malignant cardiac arrythmias while the vagus has the opposite effect. [13,14]
Chronic left ventricular dysfunction induces a hyperadrenergic state and an elevated resting HR which is a detrimental compensatory mechanism for the heart to maintain cardiac output. This chronic activation of the sympathetic nervous system associated to reduced parasympathetic (vagal) tone can increase the risk of cardiovascular events.
The Autonomic Nervous System and Physical Activity
Physical activity is a complex mulitfactorial behaviour and is influenced by various enviromental and biologiocal factors. Physical training causes physiological changes in cardio-vascular adaptation mechanisms such as higher aerobic capacity, larger stroke volumes, heart hypertrophy and bradycardia. [15-18]
Bradycardia has been described as a charactersistic feature accompanying individuals who perform regular pyhsical activity. Reported data on this topic have considered that the main mechanism responsible for bradycardia probably depends on changes in the ANS which may be due to a chronic increase in vagal activity. Furthermore, this chronic increase in parasysmpathetic tone occuring with regular dynamic exercise has been associated with an increased cardio-protective effect, particularly with a decrease in the risk of potentially lethal arrhythmias during myocardial ischemia.
Although the cardio-vascular benefits of regular physical activity are widely recognized, the accompanying ANS responses and particularly the exact mechanism responsible for the slowing of the cardiac rhythm still remain unclear and need to be fully elucidated.
One way to answer this question is to consider the different available tools allowing to assess the effects of the two branches of the autonomic function on the cardiovacular response and to apply the different measures to various populations of well-trained individuals.
Measurements of the Autonomic Nervous System
There are presently various available methods available for assessing the status of the ANS:
1) Tests based on cardio-vascular reflexes
These test include the Valsalva manoeuver, [19] the test of HR response to standing [20], and the head-upright tilt (HUT) table test. [21]
2) Biochemical tests
The degree of neurohormonal activation can be assessed by increased plasma levels of norepinephrine, [22] or endothelins. [23] An elevated activity of these tests has been recognized as a valuable predictive indicator of mortality particularly in patients with impaired left ventricular function. However, these tests are not routinely performed in daily clinical practise.
3) Scintigraphic methods
Assessment of sympathetic regional neuron density with the iodine 123 metaiodobenzylguanidine (I123 MIBG) technique is an available biological method which may assess the degree of neurohormonal activation. [24] The I123 MIBG is a guanethidine analogue that shares the same uptake, storage and release pathway as norepinephrine. The I123 MIBG imaging of the heart has made it possible to evaluate the sympathetic activity and innervation of the left ventricle. Decreased or absent myocardial I123 MIBG uptake has been described in congestive heart failure, cardiomyopathies, and MI.
Myocardial infarction produces regional cardiac sympathetic and parasympathetic denervation in the infarcted area, thus creating increased sensitivity to circulating catecholamines with dispersion of refractoriness and conduction and subsequent risk of ventricular arrhythmias. [13, 14]
4) Non invasive technics based on the ECG
The most simple ones are measurements of HR response to exercise (reserve) and HR recovery after exercise. These markers have been shown to be independent predictors of mortality. [25] Thus, the higher the HR reached during the exercise test, the better the prognosis. Concerning the values of HR recovery after exercise which mainly reflect parasympathetic reactivation researchers have reported that the rate at which the HR recovers from exercise at 1 or 2 minutes powerfully predicts prognosis, the slower the HR recovers the higher the risk of death.
In recent years, other noninvasive techniques based on the ECG have been used as markers of autonomic modulation of the heart, including HRV, [26] baroreflex sensitivity (BRS), [27] QT interval, [28] and heart rate turbulence (HRT). [29]
We will focus mainly on the value of HRV as a noninvasive method to evaluate the sympatho-vagal balance in the field of sports activity.
Heart Rate Variability and Sports Activity
Heart rate variability expresses the total amount of variations of both instantaneous HR and RR intervals, acting as a "mirror" of the cardio-respiratory system. [26, 30-32] It reflects the influence of the ANS on the sinus node of the heart.
Heart rate variability as a clinical tool provides information about sympathetic and parasympathetic autonomic function in normal and pathological hearts. [31] It may be used in different clinical settings including diabetes, [33] arterial hypertension, [34] coronary artery disease, [35-37] sudden cardiac death, [38, 39] and heart failure. [40] Furthermore, the effects of a variety of pharmacological interventions on HRV have been studied, such as antiarrhythmic drugs, [41] or anesthetics.[42] Finally, the effects of non pharmacological interventions on HRV have been analysed such as changes of position and sleep, [43] and more importantly for us the effects of physical effort, [44] and high level training [45]
It is important to point out that a large body evidence exists presently and which considers decreased global HRV as a strong predictor of increased all-cause, cardiac and/or arrhythmic mortality, particularly in patients at risk after myocardial infarction. Thus, interventions, such as physical exercise and training, that tend to improve HRV may reflect the beneficial effect they exert on the ANS.
Measurements of HRV
Measurements of HRV are generally performed on the basis of 24-hour Holter recordings or on shorter periods ranging from 0.5 to 5 minutes particularly in the field of dynamic electrocardiography. The parameters intervening in the analysis of HRV are time domain indices [46, 47] and frequency domain indices [46, 48] Time domain indices and frequency domain analysis constitute nowadays the standard clinically used parameters.
The 24-hour time domain indices are composed of statistical and geometric measures. Statistical measures, expressed in milliseconds (ms), comprise the standard deviation of all NN intervals (SDNN), the standard deviation of the averages of NN intervals in all 5-minute segments of the entire recording (SDANN), the root mean square of successive differences (RMSSD) and pNN50 (NN50 count divided by the total number of all normal RR intervals). Geometric measures include mainly the HRV triangular index (HRVi). SDNN and the HRVi are both estimates of overall HRV. Reduced SDNN and/or HRVi have been considered to reflect an increased sympathetic and a diminished vagal modulation of sinus node. [46] Conversely increased SDNN and/or HRVi reflect increased vagal tone. RMSSD and pNN50 reflect alterations in autonomic tone that are predominantly vagally mediated. [46]
Frequency domain or power spectral densitiy analysis describes the periodic oscillations of the HR signal decomposed at different frequencies and amplitudes and provides information on the amount of their relative intensity in the heart’s sinus rhythm. [46-48] Power spectral analysis is generally preformed by a nonparametric method, the fast Fourier transformation (FFT), which is characterized by discrete peaks for the several frequency components.
Spectral components are evaluated in terms of frequency given in Hertz (Hz) and amplitude assessed by the area or power spectral density of each component (given in ms2). The following spectral bands are determined: the total power, the very low frequency band (VLF), the low frequency band (LF), the high frequency band (HF), and the LF/HF ratio. Spectral components are expressed in absolute values (ms2) and in natural logarithms (ln) of the power because of the skewness of the distributions. Furthermore, LF and HF powers may also be given in normalized units (nu). Normalisation is performed by substracting from the total power the VLF component, reducing thereby the effects of noise due to artifacts and minimizing the effects of the changes in total power on the LF and HF components.
The total power of RR interval variability is the total variance and corresponds to the sum of all spectral bands. The VLF component has been identified and proposed as a marker of sympathetic activity. The LF component is modulated by both the sympathetic and parasympathetic nervous systems and thus reflects a mixture of both autonomic inputs. The HF component is generally defined as a marker of vagal modulation. The LF/HF ratio provides a measure of the global sympatho-vagal balance. Table 1 summarizes the most frequently used parameters of the time and frequency domain.
Table 1. Standard HRV measurements
|
Variable |
Unis |
Description |
Reference values46 |
|
SDNN |
ms |
standard deviation of all normal RR intervals standard deviation of the averages of normal RR intervals in all 5-minute segments of the entire recording root mean square of successive differences |
141±39 |
|
SDANN |
ms |
||
|
127±35 |
|||
|
RMSSD |
ms |
NN50 count divided by the total number of all normal RR intervals |
27±12 |
|
pNN50 |
9±7 |
||
|
% |
HRV triangular index |
||
|
variance of all NN intervals (FR: <0.4 Hz) low frequency power (FR: 0.04-0.15 Hz) high frequency power (FR : 0.15-0.4 Hz) ratio of low-high frequency power |
|||
|
HRV index |
37±15 |
||
|
TP |
ms2 |
3466±1018 |
|
|
LF |
ms2 |
1170±416 |
|
|
HF |
ms2 |
975±203 |
|
|
LF/HF ratio |
1.5±2.0 |
TP = total power; ms = milliseconds; FR = frequency range.
Effects of Physical Training on HRV
Exercise training increases HRV, suggesting a beneficial influence on cardiac autonomic activity and playing thereby a cardio-protective role. [44, 49-54] Several researchers have reported an enhanced parasympathetic tone in endurance-trained males compared with sedentary subjects, possibly in association with an attenuation of sympathetic drive. [55-58] Several months of intensive physical training in older and in younger subjects resulted in a significant increase of HRV parameters. [44] In another study training resulted in increased parasympathetic tone, reflected by higher values of the HF component. [51]
However, data on HRV remain somewhat conflicting due to a variable behavior of HRV time domain and spectral parameters. [45, 54, 59-62] Some authors [45] have observed higher time, but lower frequency domain values, particularly a lower HF component, in a group of athletes. Other authors [54] found higher SDNN in highly trained male cyclists compared to male healthy, untrained controls. However, no significant differences were observed between the study groups for RMSSD and pNN50, reflecting vagal, as well as for
the LF and HF spectral bands. In a study comparing cyclists, weight lifters and controls no significant differences in any HRV parameters were found. [61] Another study [63] aimed to investigate whether endurance-trained female athletes demonstrate differences in cardiovascular autonomic control compared with sedentary controls. Analysis of the HRV showed a longer RR interval in the trained subject but only in the spontaneous breathing condition. Conversely, athletes exhibited higher normalized LF and lower normalized HF only during the controlled breathing condition, with a subsequently higher LF/HF ratio in the trained group in the same condition.
In a recently published study by our group [64] we evaluated temporal and spectral HRV parameters determined from 24-hour continuous ECG monitoring performed during all-day activity in 40 subjects, including 12 endurance athletes, 14 hockey players and 14 untrained male volunteers (control group). As seen in Table 2, compared with controls HR values were lower and all parasympathetic-related time domain indices, including RMSSD and pNN50, as well as the LF and HF spectral components were higher in both athletes groups. However, SDNN values, which determine global HRV, were significantly higher only in endurance athletes.
Table 2. Comparisons between time and frequency domain indices in endurance athletes, team players and control group
|
Endurance athletes (n=12) |
Team players (n=14) |
Control group (n=14) |
|
|
HR (bts/min) |
 |
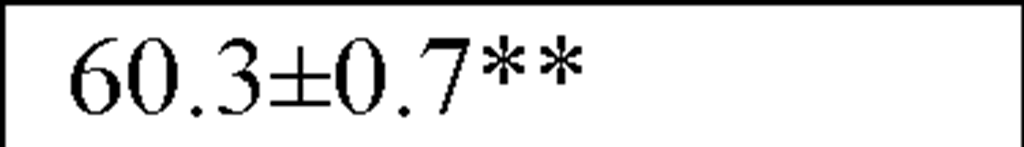 |
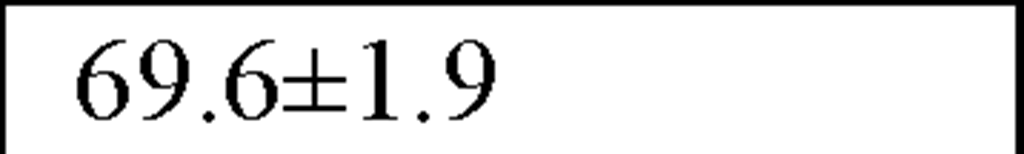 |
|
SDNN (ms) |
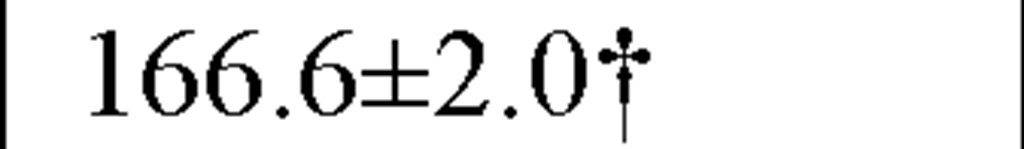 |
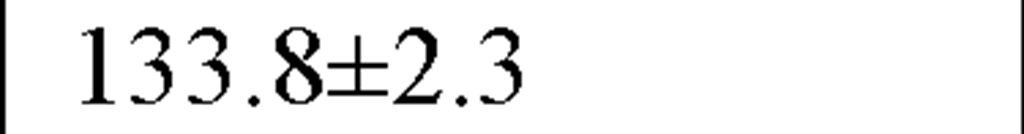 |
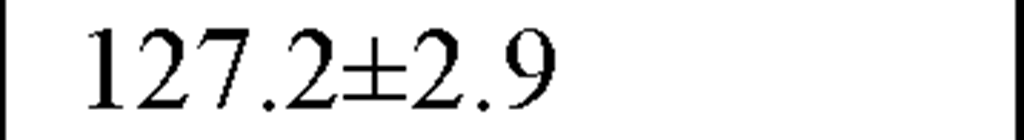 |
|
RMSSD(ms) |
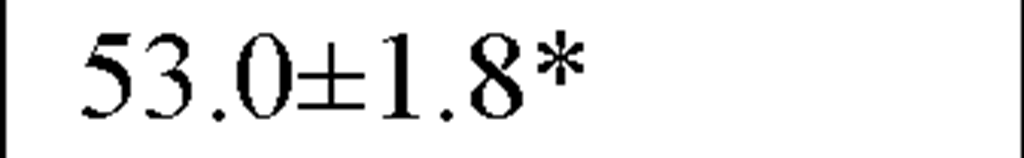 |
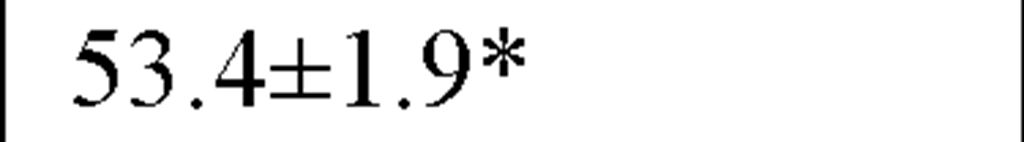 |
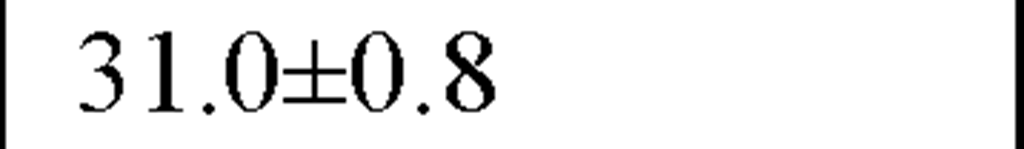 |
|
pNN50 (%) |
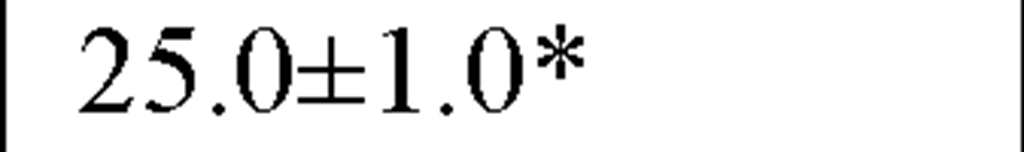 |
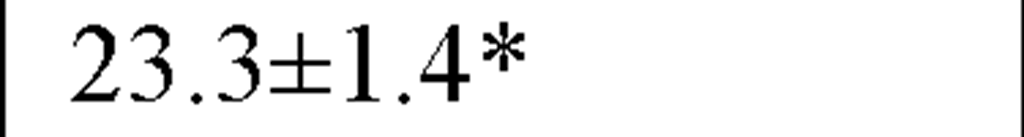 |
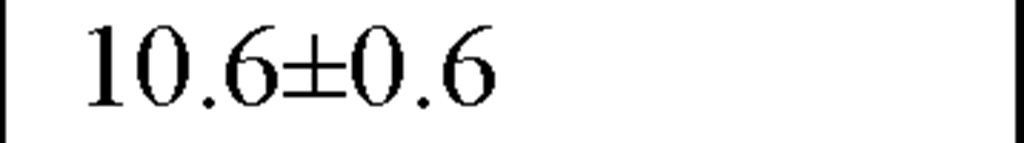 |
|
LF (ln ms2) |
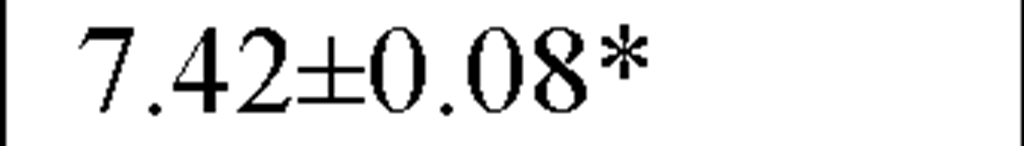 |
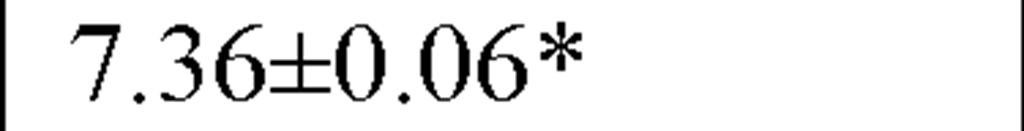 |
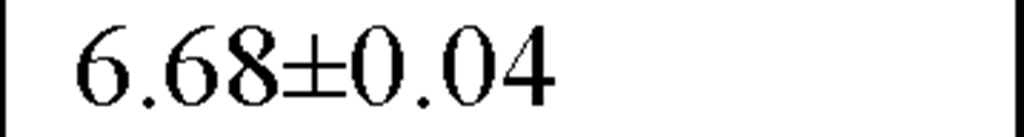 |
|
HF (ln ms2) |
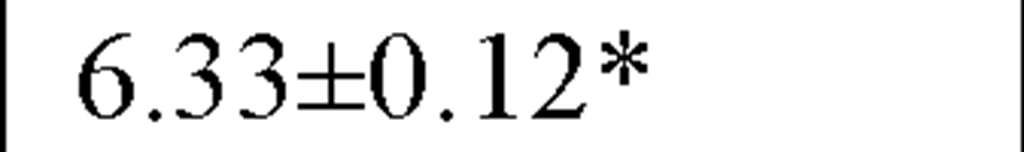 |
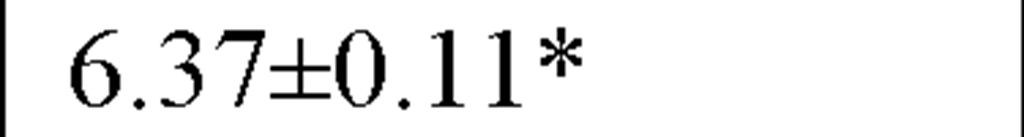 |
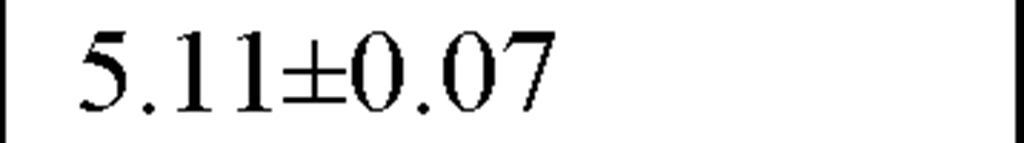 |
|
LF/HF ratio |
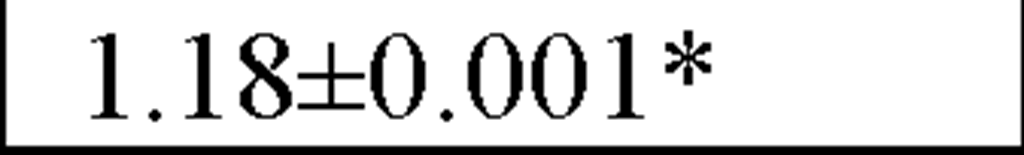 |
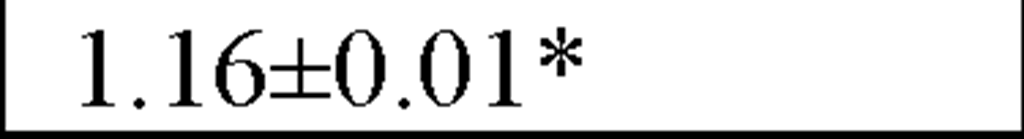 |
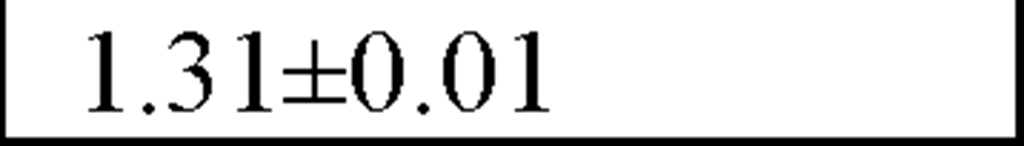 |
All values are expressed as mean±SD.
*P<0.05 and **P<0.01 when comparing endurance athletes and team players to the control group. ![]() P<0.01 when comparing endurance athletes to team players and to the control group.
P<0.01 when comparing endurance athletes to team players and to the control group.
In our study compararing different athletic disciplines we found that both athletic endurance and team playing activity had a favorable day and nighttime effect on the vagal input of the ANS, mostly reflected by increased values of pNN50 and RMSSD, by a higher HF and by a lower LF/HF ratio. Moreover, endurance athletes had higher SDNN, which is a global index of HRV, suggesting thereby that this type of sports activity may have a more substantially favorable effect on the cardiac autonomic profile.
Thus, our data indicate that both endurance and team playing sports activities influence primarily the parasympathetic tone. Endurance disciplines, such as running and cycling have a particularly beneficial effect on the global cardiac autonomic activity.