Configuration
The configuration of lesions refers to the pattern exhibited by multiple lesions within a defined area. Because the configuration of lesions may vary according to the disorder, any detectable pattern may be helpful in arriving at a definitive diagnosis. Some of the more common configurations include the following:
• Grouped or herpetiform configuration: multiple small lesions appearing within a small, defined area [see Figure 6].
• Zosteriform configuration: lesions occurring within a dermatone.
• Linear configuration: lesions oriented along a line [see Figure 7].
• Annular configuration: lesions appearing in a ringlike pattern.
• Target (iris) configuration: lesions appearing in concentric rings.
Table 2 Selected Secondary Lesions: Consensus Definitions of Dermatologic Morphologic Terms7
|
Morphologic Term |
DLP Proposed Definition |
|
Horn |
Abnormally keratinized cutaneous projection taller than it is broad |
|
Erosion |
A localized loss of the epidermal or mucosal epithelium |
|
Fissure |
A linear crack or cleavage within the skin usually found with thickened skin |
|
Ulcer |
A circumscribed loss of the epidermis and at least the upper dermis; ulcers are further classified by their depth, border/shape, edge, and tissue at their base |
Figure 5 (a) Schematic drawing of a skin ulceration. A skin ulceration is a circumscribed lesion denuded of epidermis and at least some dermis. (b) A well-defined 3.5 by 4.0 cm ulceration with an erythematous granulating base is present in a patient who has early evolving pyoderma gangrenosum.
• Arcuate configuration: lesions appearing in a semicircular pattern.
• Polycyclic configuration: lesions appearing as interlocking rings.
• Serpiginous configuration: lesions appearing in snakelike whorls.
• Digitate configuration: lesions resembling the size and shape of a fingertip.
When lesions coalesce over large areas, they are termed confluent. Erythroderma describes a widespread confluence of rash covering nearly all of the cutaneous surface.
Color
The color of cutaneous lesions also provides important diagnostic clues. Lesions may be flesh-colored, hyperpigmented or hypopigmented, erythematous, or virtually any color of the rainbow. Purpuric rashes caused by the extravasation of red blood cells show no blanching on diascopy (i.e., a test in which a glass slide or lens is pressed against the skin).
Categories of Skin Diseases
The appearance of individual lesions on the skin (e.g., primary lesions and their secondary changes) classifies a rash or growth within a major category of skin disease. The most common skin diseases and many important rare conditions can be classified into one of five disease categories on the basis of their characteristic lesions. Once the category is determined, the diseases within that category are considered in the differential diagnosis of the presenting disorder [see Table 4].
As a clinician’s dermatologic knowledge becomes more sophisticated, additional categories can be mastered, including (but not limited to) diseases of the hair, nails, or mucous membranes; photosensitivity diseases; diseases of vascular reactivity; ulcerative skin conditions; and conditions typical of specific distributions, such as diseases of the genitalia, feet and hands, and eyelids. Manuals of differential diagnosis based on the morphology of lesions and other physical features are plentiful and can be quite helpful in determining a diagnosis.
Table 3 Other Important Morphologic Terms: Consensus Definitions of Dermatologic Morphologic Terms7
|
Morphologic Term |
DLP Proposed Definition |
|
Abscess |
A localized accumulation of pus in the dermis or subcutaneous tissue; frequently red, warm, and tender |
|
Atrophy |
A thinning of tissue defined by the location (e.g., epidermal atrophy, dermal atrophy, or subcutaneous atrophy) |
|
Burrow |
A threadlike linear or serpiginous tunnel in the skin typically made by a parasite |
|
Carbuncle |
An inflammatory nodule composed of coalescing furuncles |
|
Ecchymosis |
A discoloration of the skin or mucous membranes resulting from extravasation of blood that exhibits color change over time; the characteristic transition is from blue-black to brown-yellow to green |
|
Erythema |
Localized, blanchable redness of the skin or mucous membranes |
|
Exfoliation |
Desquamation of the superficial epidermis appearing as a fine scaling or as peeling sheets |
|
Furuncle |
A follicle-centered nodule caused by a suppurative infection characterized by pain, redness, and perhaps visible pus; usually greater than 1 cm in diameter |
|
Induration |
Hardening of the skin beneath the epidermis, usually caused by edema, dermal sclerosis, inflammation, or infiltration |
|
Petechiae |
Purpuric nonblanchable macules resulting from tiny hemorrhages, initially measuring 1 to 2 mm |
|
Poikiloderma |
An area of variegated pigmentation, atrophy, and telangiectasia |
|
Purpura |
Hemorrhaging into skin or mucous membranes that varies in size, color, and duration; types of pur-pura include palpable purpura, ecchymosis, and petechiae |
|
Telangiectasia |
Visible, persistent dilation of small, superficial cutaneous blood vessels |
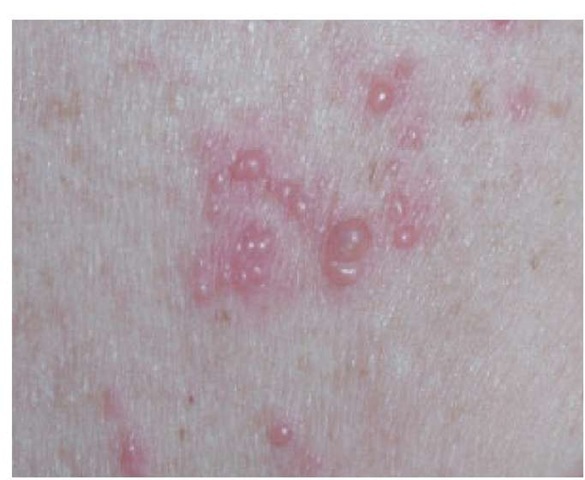
Figure 6 Close-up view of a herpetiform pattern of vesicles on an erythematous base within a dermatome in a patient with herpes zoster.
Arriving at a Diagnosis
It is important to begin the assessment of a skin condition with a broad differential diagnosis, noting the presentation as characteristic of one of the categories of skin disease [see Table 4]. Using physical findings, patient history, and diagnostic testing, the differential diagnosis is gradually narrowed until a diagnosis is determined. For example, scaling conditions, including rashes composed of both papules and plaques, are characterized as papulosquamous skin diseases; each papulosquamous condition [see Table 4] should be considered in the differential diagnosis of a scaling rash. The specific features of each of the papu-losquamous conditions are compared with the patient’s lesions to systematically identify the disorder. It is critical that the initial differential diagnosis be broadly determined. Jumping to an early conclusion and not systematically considering all of the possible papulosquamous disorders can result in an incorrect diagnosis. In fact, if the actual diagnosis is not among the diseases ini-tially considered, it is much more difficult to determine the correct diagnosis.
Figure 7 Linear arrangement of papules in a patient with contact dermatitis caused by poison ivy.
Table 4 Categories of Skin Disease
|
Papulosquamous diseases (discrete papules or plaques with scaling) |
Psoriasis vulgaris |
|
Chronic atopic dermatitis |
|
|
Lichen planus |
|
|
Pityriasis rosea |
|
|
Fungal infections |
|
|
Secondary syphilis |
|
|
Mycosis fungoides |
|
|
Blistering diseases (vesicles, bullae, pustules) |
Acute allergic contact dermatitis |
|
Bullous pemphigoid |
|
|
Pemphigus vulgaris |
|
|
Dermatitis herpetiformis |
|
|
Herpesvirus infections |
|
|
Bacterial folliculitis |
|
|
Nonscaling erythematous (macules, patches, wheals) and infiltrative diseases (plaques) |
Urticaria |
|
Morbilliform drug eruptions |
|
|
Viral exanthems |
|
|
Sarcoidosis |
|
|
Leukemia and lymphoma cutis |
|
|
Amyloidosis |
|
|
Diseases of pigmentation (macules or patches of various colors) |
Vitiligo |
|
Tinea versicolor |
|
|
Pityriasis alba |
|
|
Cafe au lait macules |
|
|
Lentigines |
|
|
Benign and premalignant tumors (macules, papules, nodules, tumors) |
Actinic keratosis |
|
Basal cell carcinoma |
|
|
Squamous cell carcinoma |
|
|
Melanoma |
|
|
Acrochordons |
|
|
Dermatofibroma |
|
|
Neurofibroma |
|
|
Melanocytic nevi |
|
|
Adnexal tumors |
Diagnosis is almost always more difficult than treatment. Consultation with a dermatologist is recommended when the diagnosis is uncertain, particularly in cases in which treatment may fail or may lead to iatrogenic disease. The dermatologist may help define the primary lesions that permit the accurate categorization of the disease process and, in turn, suggest the diagnosis.
If a diagnosis remains in doubt, a follow-up visit with the patient should be scheduled because, as the disease progresses, the development of primary lesions and lesion distribution may make the diagnosis more apparent. In addition, single, confirmatory tests often prove helpful in the diagnosis of cutaneous presentations; tests used to confirm a diagnosis include a Wood light examination, potassium hydroxide (KOH) preparation, sampling for fungal culture, scabies preparation, Tzanck preparation, patch testing, skin biopsy, dark-field microscopic examination, microscopic hair-shaft analysis, Gram stain, and viral or bacterial cultures.
A Wood light examination is performed by shining a black light on the skin in a dimly lit room. Epidermal pigmentation (e.g., lentigines) is highlighted by this examination, whereas dermal pigmentation (e.g., Mongolian spot) disappears. A search for depigmented spots such as ash-leaf macules in babies with tuberous sclerosis is also aided by the Wood lamp.
A KOH test for fungal infections involves applying KOH to scales of skin or hair shafts to clear the keratin so that fungal hyphae and spores can be identified. For example, scales can be lightly scraped onto a glass slide after placing the slide on the advancing margin of an annular plaque with central clearing. After a coverslip is applied, 2.5% KOH preparation is applied to the slide next to the coverslip. The KOH preparation spreads under the coverslip by capillary action. After gentle heating, excess KOH is blotted away, and the specimen is examined under a microscope. Fungal infections can also be confirmed by obtaining scales by lightly scraping papulosquamous lesions and sprinkling the scales onto Sabouraud dextrose agar. This agar preparation is then incubated at room temperature for several weeks, after which it is analyzed for colony growth, color, and morphology.
A scabies preparation test involves applying oil to excoriated lesions—frequently found on wrists and finger webs—and lightly scraping the burrows to obtain their contents. The scrapings are placed on a slide with coverslip; the test is positive if scabies mites, eggs, or feces are visible on microscopic examination.
Tzanck preparations are smears obtained from the base of intact vesicles and stained with one of a variety of nuclear stains. A finding of multinucleated giant cells suggests a diagnosis of herpes simplex or herpes zoster infection.
Patch testing is performed to objectively elucidate the specific cause of an allergic contact dermatitis. Standard allergens are applied under patches for 24 hours, and the reactions are read 48 hours and 1 week later.
Skin biopsies are helpful in confirming the diagnosis of a variety of inflammatory and neoplastic diseases. Dark-field microscopic examination of serous fluid from genital ulcers identifies spirochetes in lesions of primary syphilis. Hair-shaft analysis is helpful when alopecia is caused by hair-shaft abnormalities. Finally, viral and bacterial cultures using specific swabs can provide laboratory confirmation of a variety of viral and bacterial diseases.