Prevention: A Brief Overview
During the past 2 decades, disease and injury prevention has occupied an expanding share of medical practice. Public interest in prevention is very high, driven by a steady accumulation of high-quality evidence that preventive interventions do reduce cause-specific death rates. The purpose of these interventions is to eliminate the root causes of diseases that precede death (e.g., heart disease, cancer, and stroke), which in the United States in 1990 were tobacco use (400,000 deaths), poor diet and inadequate physical activity (300,000 deaths), alcohol consumption (100,000 deaths), microbial agents (90,000 deaths), toxic agents (60,000 deaths), firearms (35,000 deaths), unprotected sexual intercourse (30,000 deaths), motor vehicle accidents (25,000 deaths), and use of illicit drugs (20,000 deaths).1 These causes of death are the targets of disease and injury prevention. They contribute to 50% of the deaths in the United States. Most are simply bad habits, and changing those habits reduces the risk of dying.
Physicians have two principal roles in prevention: they identify risk factors for disease and injury, and they act as teachers and counselors. Physicians must expand their routine questioning beyond diet, exercise, and substance abuse to include recreational activities that increase the risk of death (e.g., boating, bicycling, and riding motorcycles), gun ownership, use of swimming pools, smoke detectors in the home, and domestic violence. In counseling patients about a healthy diet (including vitamin supplements), exercise, and other elements of a healthy lifestyle, physicians must often help patients adopt healthy living habits. Some patients simply require reinforcement of a chosen lifestyle. Others need help in changing harmful habitual behaviors to healthy behaviors.
The report of the second United States Preventive Services Task Force (USPSTF)2 contains evidence-based guidelines on 70 prevention topics [see Table 1]. As they become available, the third USPSTF reports will appear on its Web site (http://www.ahcpr.gov/clinic/cps3dix.htm). Other literature is also helpful [see CE:IV Diet and Exercise, CE:V Adult Preventive Health Care, 7:XXXIII HIV and AIDS, 13:111 Alcohol Abuse and Dependency, and 13:VI Drug Abuse and Addiction].
Caveats in disease and injury prevention
Although disease and injury prevention can have a significant effect on the health of the public, physicians should observe several caveats. First, the baseline risk of most diseases is very low in the average person. Each year, colon cancer occurs in 165 per 100,000 men 60 to 64 years of age. The low baseline risk means that the number needed to screen or treat to prevent one death is often very high. Annual fecal occult blood testing must be performed on more than 300 people for 12 years to prevent one death from colon cancer. Whether this inefficiency is important depends partly on the cost of the intervention. Fecal occult blood testing can be costly because it must be performed annually and because abnormal results trigger costly diagnostic tests. Seat belts and smoke alarms are very cost-effective because they incur a onetime cost.
Second, disease prevention does not prevent death. At best, it postpones death by shifting the cause of death from the targeted disease to another disease that strikes later in life. In the Minnesota Colon Cancer Control Study, a randomized trial of fecal occult blood testing, annual testing reduced deaths from colon cancer during 18 years of surveillance. However, the total mortality was the same in the control group and the intervention groups. Our preventive efforts may reduce the likelihood of death from the target disease, whose identity and natural history we know. Inevitably, we raise the lifetime probability of dying from another disease.
|
Table 1 Recommendations of the United States Preventive Services Task Force2 |
|
Tobacco Use |
|
Provide tobacco cessation counseling to patients who use tobacco products. Counsel pregnant women and parents about the potentially harmful effects of smoking on fetal and child health. Prescribe nicotine patches or gum to selected patients as an adjunct to counseling. Give antitobacco messages to young people as part of health promotion counseling. |
|
Alcohol Abuse Screen all adults and adolescents for problem drinking, using a careful history or a standardized screening questionnaire. Advise pregnant women to limit or abstain from drinking. Counsel all persons who use alcohol about the dangers of operating a motor vehicle or engaging in other potentially dangerous activities while drinking. |
|
Drug Abuse* Although the evidence is insufficient for a strong recommendation to be made, it is reasonable to ask adolescents and adults about drug use and drug-related problems. All pregnant women should be advised of the potential adverse effects of drug use on fetal development. Refer drug-abusing patients to specialized treatment facilities where available. |
|
Preventing Motor Vehicle Injuries Counsel all patients and the parents of young people to use occupant restraints (lab/shoulder safety belts and child safety seats), to wear helmets when riding motorcycles, and to refrain from driving while under the influence of alcohol or other drugs. |
|
Preventing Falls* Counsel elderly patients on specific measures to reduce the risk of falls. Effective measures include exercise, balance training, environmental hazard reduction, and monitoring and adjusting medications. Provide multifactorial individualized interventions to elderly patients at especially high risk for falls. |
|
Fires Advise homeowners to install smoke detection devices and test them periodically. Infants and children should wear flame-resistant nightclothes. Smokers should cease or reduce smoking. |
|
Drowning Families with swimming pools should install four-sided 4-ft isolation fences with self-latching gates. |
|
Firearm Injuries Remove firearms from the home or store them unloaded in a locked compartment. |
*There is insufficient evidence to recommend routine screening for drug abuse with standardized questionnaires or biologic assays.
+There is insufficient evidence to recommend for or against counseling patients to avoid pedestrian injuries.
*There is insufficient evidence of effectiveness of external hip protectors.
Third, we know little about the age at which we should stop our efforts to prevent disease. Our studies provide good information on effectiveness in the study population, which is usually in middle age, but we do not know how the results apply to older people, whose care will occupy an increasing amount of the primary care physician’s time.3 Interventions that take years to show their impact may be ill suited to people whose life expectancy is measured in years rather than decades.
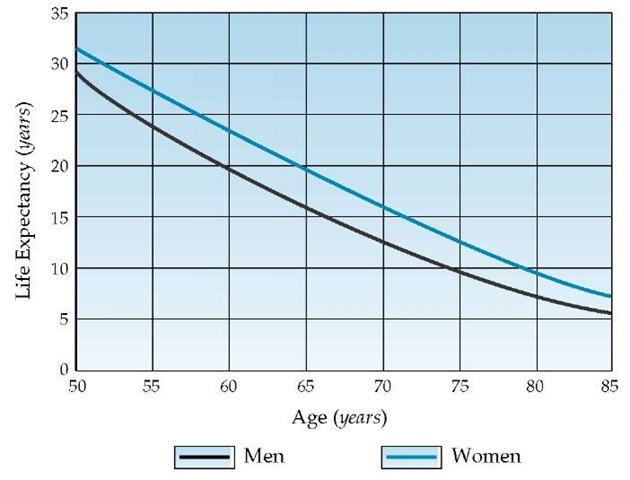
The decision to do a screening test on an older person should depend on the person’s general health, which may be quantified as the person’s physiologic age. The physician can determine a patient’s physiologic age by asking the patient to rate his or her health as excellent, good, fair, or poor.3 The most likely age at death is the sum of the patient’s actual age and the life expectancy that corresponds to the patient’s physiologic age. For example, a 75-year-old man in excellent health has a physiologic age of 67 years, which corresponds to a 14.7-year life expectancy [see Figure 1]. The most likely age at death is 75 years plus 14.7 years, or 90 years. This information can be very helpful in deciding how hard to press preventive efforts. With a life expectancy of almost 15 years, a 75-year-old man has plenty of time in which to experience gains from preventive efforts.
Changing behavior
Many interventions of proven efficacy are not completely effective because patients are reluctant to change long-established risky behaviors. The USPSTF recommends the following steps for helping patients use their ability to change (self-efficacy)4:
1. Match teaching to the patient. Identify a patient’s beliefs about a behavior, and adjust advice to the patient’s lifestyle. Building the patient’s confidence in his or her ability to change requires recognizable successes; define success in terms of goals the patient can achieve.
2. Tell why, what, and when. Patients need to know the reason for a recommendation and the results of following the recommendation. They must also know the time scale for the results so that they do not become discouraged when results do not occur immediately.
3. Small changes succeed. As the patient achieves small successes, propose larger but achievable goals.
4. Be specific. Couch suggestions in terms of current behavior, and give precise instructions in writing.
5. Add new behaviors. Adopting good habits is often easier than discarding bad ones.
6. Link positive behaviors with the daily routine. For example, patients can be encouraged to exercise before lunch or to take medication immediately after brushing teeth.
7. Do not mince words. Tell the patient directly, simply, and specifically what you want and why.
8. Extract promises. Get explicit commitments from the patient. Have the patient tell you exactly how he or she will achieve a goal. Assess the patient’s self-confidence and address concerns about succeeding.
9. Use combination strategies. An approach that combines several strategies is more likely to succeed than a single strategy.
10. Involve others. Members of the physician’s office staff can become educators. Anyone can offer encouragement to patients.
Figure 1 Life expectancy of men and women in the United States.
11. Refer. Subspecialists in many chronic diseases have trained teams that can educate patients far more effectively than individual physicians can. Another form of referral is sending novice patients to talk with successful patients.
12. Stay interested. According to research findings, a call from a health professional to inquire about progress is very effective in changing a behavior. A well-organized office will have a protocol for making these calls a matter of routine.
Health Risks from Substance Abuse
Substance abuse exacts a large toll on the health of the American people, accounting for at least 520,000 deaths in 1990, or 24% of all deaths.1 Unfortunately, many physicians do not place diseases resulting from self-abuse in the same category as diseases that strike seemingly by chance. Two factors make helping patients shed their habitual use of tobacco, alcohol, and illicit drugs a very efficient way for physicians to add healthy years to patients’ lives. First, there is a high baseline risk that substance abuse will lead to serious disease. Therefore, the absolute reduction in risk from a successful intervention is high. This principle is especially true of substance abuse during pregnancy. Second, substance abuse is primarily a problem of youth and middle age, so a successful intervention can add many years of healthy life.
Tobacco use
Tobacco contains an addictive drug, nicotine, as well as other substances that contribute to death from cardiovascular disease, cancer, and chronic lung disease. Smoking also contributes to 10% of infant deaths and 20% to 30% of low-birth-weight infants.5 Tobacco use contributed to one in every five deaths in the United States in 1990 (420,000 deaths a year). In one 40-year cohort study of male physicians in the United Kingdom, half of the deaths after age 35 were smoking related, and smoking caused 25% of the residential fires that resulted in death.5 Tobacco use is less common than it was several decades ago, but 25% of adults smoke, and an increasing number of smokers are women. Women are starting to smoke earlier— many as high-school students—and they are heavier smokers; nearly twice as many women smoked at least 25 cigarettes a day in 1985 as in 1965.6
Cigarettes are highly addictive. Fewer than 10% of people who quit smoking for a day are still abstinent 1 year later. Nicotine, like other highly addictive substances, acts on the dopaminergic mesolimbic pathway, the brain reward pathway that controls motivated behaviors [see 13:VI Drug Abuse and Addiction]. The use of nicotine is self-reinforcing, leading to compulsive use. Nicotine produces a withdrawal syndrome that begins within a few hours of abstinence, peaks within the first week, and continues for several weeks. The withdrawal syndrome includes dysphoria, insomnia, irritability, anxiety, difficulty in concentrating, restlessness, slowed heart rate, and increased appetite.7
Detection of cigarette smoking is easy; most smokers are truthful when asked about their habit and its extent, and the odor of tobacco is an additional diagnostic clue.
Smoking cessation reduces mortality dramatically. The risk of some diseases (e.g., myocardial infarction and stroke) declines rapidly within a few years after quitting [see Table 2].8 This information is important when one is trying to convince long-term smokers to quit.
Research has shown that a strong message from a personal physician is the most important factor in successful quitting. The elements of successful quitting are consistent, repeated, and strong advice to stop smoking; setting a specific quit date; and follow-up visits to reinforce behavior [see Table 3]. However, not all physicians counsel smokers to quit. In one study, only 78% of cigarette smokers reported that their physician had advised them to quit.9
A current theory in behavioral psychology suggests that changes in behavior reflect predictable stages in the readiness to change, ranging from no intention to change, to definite plans to change in the near future, to active attempts at change. A stage of readiness to change is predictive of quitting,10 and this behavioral model may help clinicians shape smoking-ces-sation efforts to the patient’s state of mind.
School-based prevention has received extensive study, and it is effective for at least 2 to 4 years. Clinicians, especially those caring for adolescents, must reinforce the messages of school-based programs.
Nicotine products are an important adjunct to counseling.11 Drugs are most reinforcing when the level in the brain rises very rapidly, as with inhaled nicotine. Nicotine in medication form, especially transdermal products, appears in the blood much more slowly than inhaled nicotine and produces much less of the reinforcing effect that leads to craving for cigarettes. Plasma nicotine concentrations after transdermal administration reach stable levels in 2 to 3 days. Nicotine medications reduce the symptoms of withdrawal, so that symptoms in the first week are reduced to the level of symptoms at 5 to 10 weeks. Nicotine medications may also provide some nicotinelike effects, such as helping patients to sustain concentration and deal with stress.
Nicotine medications improve abstinence rates, but abstinence at 1 year is still the exception. A meta-analysis summarized the results of 46 trials of nicotine gum and 20 trials of nicotine patches.12 At 12 months, 19% of patients who received nicotine gum were abstinent, as compared with 11% of patients who did not receive gum. The number needed to treat to achieve one success at 1 year (NNT) was 17 (P < 0.001). Transdermal nicotine led to similar rates. At 12 months, 16% of patients who received a transdermal nicotine patch had quit smoking, as compared with 9% who did not receive the patch (NNT, 16).
Table 2 Years of Smoking Abstinence Needed to Reduce Risk of Disease
|
Disease |
Years until Risk Is Half of a Current Smoker’s Risk |
Years until Risk Is Equal to a Never-smoker’s Risk |
|
Recurrent myocardial infarction or death from coronary artery disease |
1 |
15 |
|
Stroke |
2-4 |
5-15 |
|
Oral and esophageal cancer |
5 |
— |
|
Lung cancer |
10 |
20 |
Clonidine also increases the rate of abstinence at 12 months. Weight gain is a common occurrence in patients who have stopped smoking. The average weight gain in a national sample of adults who had stopped smoking was 4.4 kg for men and 5.0 kg for women.13
The dose of nicotine medications should depend on the degree of nicotine dependence.11 The score on the Fagerstrom questionnaire14 and the number of cigarettes a day are measures of dependence. Follow-up calls at prearranged times will help the patient to maintain abstinence. It is best to designate a specific member of the physician’s office staff to be the smoking-cessation coordinator.
The starting dose of nicotine gum (nicotine polacrilex) is 2 mg per two cigarettes; in patients who smoke more than 20 cigarettes a day, the dose should be 4 mg per three or four cigarettes. Patients may take additional unit doses if their withdrawal symptoms are unpleasant. The medication should be taken at regular intervals throughout the waking hours. The patient should compress the gum a few times with the teeth and then hold it in the mouth, repeating the cycle every minute or so for 15 to 30 minutes for each dose. After 1 to 2 months, weaning can begin with a reduction of 1 unit dose a week.
With transdermal nicotine, patients who smoke more than 10 cigarettes a day should use the largest patch (21 mg). After 1 to 2 months, weaning can begin with each of the lower doses (usually 14 mg and 7 mg, respectively), prescribed for 2 to 4 weeks. Patients who smoke fewer than 10 cigarettes a day can start with the 14 mg dose. A hairless site allows the best absorption. The patient should rotate sites to avoid skin irritation.
Nicotine medications are quite safe11—certainly safer than cigarette smoking—even for patients with cardiovascular disease. The only contraindication is hypersensitivity to nicotine or to a component of the delivery system. Twenty-four-hour application of transdermal medication can result in sleep disturbance, which subsides if the medication is removed before sleep.
|
Table 3 Elements of a Successful Smoking Cessation Strategy |
|
Direct, face-to-face advice and suggestions |
|
Reinforcement, especially in first 2 weeks |
|
Office reminders: a sticker on chart of smokers may stimulate physician to deliver antitobacco message at each visit |
|
Self-help materials |
|
Community programs for additional help |
|
Drug therapy |
Nicotine medication during pregnancy is of concern but probably of less concern than heavy smoking during pregnancy. Medication during pregnancy should be reserved for women who have failed to quit without medication and who smoke more than 10 to 15 cigarettes a day. Dependence on nicotine medications is most likely with delivery systems such as a nasal spray, which causes a rapid rise in the plasma nicotine concentration, and a small number of patients will still be using nicotine medication 1 year after starting treatment.
Nicotine therapy is not the only pharmacologic approach to smoking cessation. Another approach focuses on dopamine. Nicotine releases norepinephrine in the brain and increases dopamine in areas of the brain associated with reinforcing the effects of addictive substances, such as opioids. Bupropion potentiates the effect of norepinephrine and dopamine by acting as a weak inhibitor of their neuronal uptake. Thus, bupropion can mimic some of the central nervous system effects of nicotine and act as a substitute for nicotine in people who are trying to quit cigarettes. Randomized clinical trials have shown that abstinence rates are approximately twice as high with bupropion as with placebo.15 In one trial, for example, the rates of abstinence from tobacco at 1 year were 12% for those taking placebo and 23% for those taking 150 or 300 mg of bupropion.16 Side effects of bupropion include agitation and insomnia. Seizures are very uncommon when the daily dose of bupropion is 300 mg or less.
The recommended dose of bupropion is 150 mg/day for the first 3 days and then 150 mg twice daily. The patient should wait to stop smoking until he or she has been on bupropion for 1 week. There are no peer-reviewed reports comparing nicotine-replacement products with bupropion or detailing possible synergy between the two drugs.