Pulmonary Features
Pulmonary involvement can be documented in most patients with SSc and is now the leading cause of death. The two main types of significant pulmonary involvement are ILD and PAH; many patients develop some degree of both complications. Less frequent pulmonary manifestations include aspiration pneumonitis complicating gastroesophageal reflux, pulmonary hemorrhage due to endobronchial telangiectasia, obliterative bronchiolitis, pleural reactions, restrictive ventilatory defect due to chest wall fibrosis, and spontaneous pneumothorax. The incidence of lung cancer, particularly bronchoalveolar carcinoma, may be increased in patients with SSc.
Pulmonary involvement may remain asymptomatic until it is advanced. The most frequent presenting symptoms of pulmonary involvement—exertional dyspnea, fatigue, and reduced exercise tolerance—are often subtle and slowly progressive.
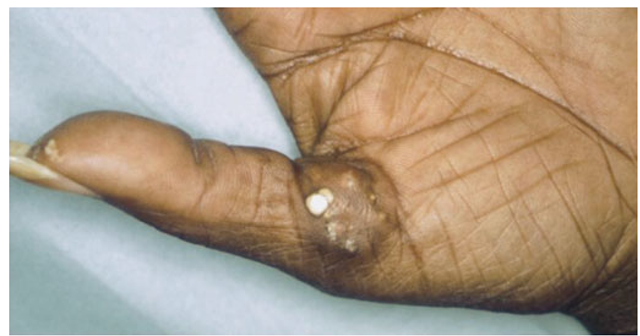
FIGURE 7-6
Calcinosis cutis. Note large calcific deposit breaking through the skin in a patient with limited cutaneous SSc.
A chronic dry cough may be present. Physical examination may reveal “Velcro” crackles at the lung bases. Pulmonary function testing (PFT) is a sensitive method for detecting early pulmonary involvement in asymptomatic patients. The most common abnormalities are reductions in forced vital capacity (FVC) or single breath diffusing capacity (DLCO). A reduction in DLCO that is significantly out of proportion to the reduction in FVC suggests pulmonary vascular disease, but may also be due to anemia. With exercise, patients show a decrease in PO2.
Interstitial Lung Disease (ILD)
Some evidence of ILD can be found at autopsy in up to 90% of patients with SSc and by thin-section highresolution computed tomography (HRCT) in 85%. ILD and pulmonary fibrosis cause restrictive lung disease with impaired gas exchange, characterized on PFT by decreased FVC and DLCO but unaffected flow rates. Clinically significant ILD develops in 16-43% of patients with SSc, the frequency depending on the detection method used and the characteristics of the patient population. Risk factors include male gender, African-American race, diffuse skin involvement, severe gastroesophageal reflux, and the presence of topoisomerase-I autoantibodies, as well as a low FVC or DLCO at initial presentation. In patients who develop significant ILD, the most rapid progression in lung disease occurs early in the course of the disease (within the first 3 years), when the FVC declines by an average of 32% per year.
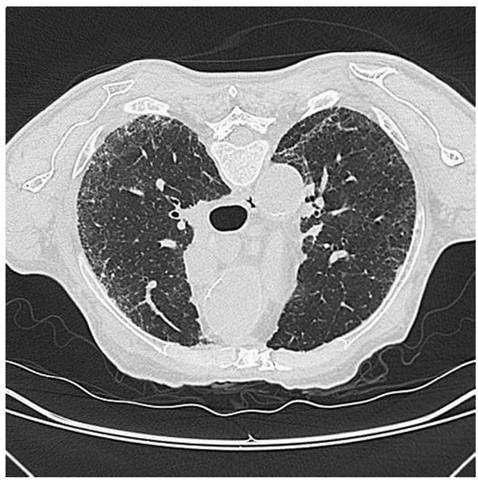
Chest radiography is useful for ruling out infection and other causes of pulmonary involvement, but it is relatively insensitive for detection of early ILD. HRCT of the chest is more sensitive and may show reticular linear opacities predominantly in the lower lobes, even in asymptomatic patients (Fig. 7-7).Additional findings include mediastinal lymphadenopathy, nodules, and honeycombing. Ground-glass opacification, seen in 50% of patients, is not specific for identifying alveolitis or predicting rapidly progressing lung disease. Bronchoalveolar lavage (BAL) may be useful for identifying inflammation in the lower respiratory tract and ruling out infection. In some studies, an elevated proportion of neutrophils (>2%) and/or eosinophils (>3%) in the BAL fluid was associated with more extensive lung disease, more rapid decline in FVC, and reduced survival. Lung biopsy is indicated only in patients with atypical findings on chest radiographs and should be thoracoscopically guided. The histologic pattern on lung biopsy may be helpful in predicting the risk of progression of ILD. The most common pattern in SSc, nonspecific interstitial pneumonitis, carries a better prognosis than usual interstitial pneumonitis. Recent studies suggest that measurement of serum markers such as KL-6, a glycoprotein found in type II pneumocytes and alveolar macrophages, may have utility in the detection and serial monitoring of ILD in patients with SSc.
FIGURE 7-7
High-resolution CT scan of the lungs. Note peripheral bilateral reticulonodular opacifications in the lower lobes of the lungs in a patient with diffuse cutaneous SSc.
Pulmonary Arterial Hypertension (PAH)
PAH, defined as a mean pulmonary arterial pressure >25 mmHg at rest, as determined by right heart catheterization, is increasingly recognized as a major complication of SSc.Approximately 12-25% of SSc patients have evidence of PAH. In these patients, PAH may occur in association with ILD or as an isolated pulmonary abnormality. The natural history of SSc-associated PAH is variable, but in many patients it follows a relentlessly downhill course with development of right heart failure and significant mortality. Risk factors for PAH include limited cutaneous disease with anticentromere antibodies, late age at disease onset, severe Raynaud’s phenomenon, and the presence of U1-RNP, U3-RNP (fibrillarin), and B23 antibodies.
Patients with early PAH are generally asymptomatic. The initial symptom is typically exertional dyspnea and reduced exercise capacity. With progression, angina, exertional near-syncope, and symptoms and signs of right-sided heart failure appear. Physical examination shows tachypnea, a prominent pulmonic S2 heart sound, palpable right ventricular heave, elevated jugular venous pressure, and dependent edema. Doppler echocardiography provides an estimate of pulmonary arterial systolic pressures and also indicates the presence of valvular abnormalities or left ventricular systolic or diastolic dysfunction that could cause pulmonary hypertension due to elevated pulmonary venous pressures. Echocardiogram-derived estimates of pulmonary arterial systolic pressures exceeding 40 mmHg at rest suggest PAH. Pulmonary function testing may show a reduced DLCO in isolation or combined with a restrictive pattern. Right heart catheterization is required to confirm the presence of PAH and accurately assess its severity. Recent studies indicate that elevated serum levels of brain natriuretic peptide (BNP) and N-terminal BNP correlate with the presence and severity of PAH, suggesting a potential role for BNP measurements in screening SSc patients for PAH and in monitoring response to treatment. The prognosis of PAH is determined by the degree of pulmonary arterial pressure elevation.
Gastrointestinal Involvement
The gastrointestinal tract is affected in up to 90% of patients with SSc and may be asymptomatic or present with unexplained weight loss. Gastrointestinal involvement is characterized by abnormal motility of the esophagus, stomach, and small and large intestines. The pathological features are similar throughout the length of the gastrointestinal tract, with prominent atrophy and fibrosis of smooth muscle, intact mucosa, and obliterative small-vessel vascu-lopathy. Oropharyngeal manifestations are frequent and are due to a combination of xerostomia, reduced oral aperture, and periodontal disease. Symptoms of gastroesophageal reflux disease (GERD) develop early. Most patients have heartburn, regurgitation, and dysphagia. A combination of reduced lower esophageal sphincter pressure, impaired esophageal clearance of refluxed gastric contents due to diminished motility in the distal two-thirds of the esophagus, and delayed gastric emptying accounts for GERD. Severe erosive esophagitis may be found on endoscopy in patients with minimal symptoms. Endoscopy may be necessary to rule out opportunistic infections with Candida, herpes virus, and cytomegalovirus. Esophageal strictures and Barrett’s esophagus may complicate chronic GERD. Because Barrett’s esophagus is associated with adenocarcinoma, SSc patients with this lesion need to undergo periodic endoscopy and biopsy. Extra-esophageal manifestations of GERD, such as hoarseness and chronic cough, and aspiration pneumonitis aggravating ILD may occur.
Gastroparesis is common and may cause early satiety, abdominal pain and distension, and aggravated reflux symptoms. The presence and severity of gastroparesis can be assessed by radionuclide gastric emptying studies. Gastric vascular ectasia may occur in the antrum. These subepithelial lesions, part of the diffuse small-vessel vas-culopathy of SSc, give a watermelon appearance on endoscopy. Patients with watermelon stomach may have recurrent episodes of occult gastrointestinal bleeding, resulting in unexplained anemia. Manometric testing shows abnormalities in the upper small intestines of most patients with SSc. Impaired motility may result in malabsorption and chronic diarrhea secondary to bacterial overgrowth. Fat and protein malabsorption and vitamin B12 and vitamin D deficiency ensue, sometimes culminating in severe malnutrition. Disturbed intestinal motor function can also cause intestinal pseudoobstruction. Patients present with recurrent episodes of acute abdominal pain, nausea, and vomiting. Radiographic studies show acute intestinal obstruction, and the major diagnostic challenge is to differentiate pseudoobstruction, which responds to supportive care and intravenous nutritional supplementation, from mechanical obstruction. Colonic involvement may cause constipation, fecal incontinence, and rectal prolapse. In late-stage SSc, wide-mouth sacculations in the colon may occur, causing perforation and bleeding. An occasional radiologic finding is pneumatosis cystoides intestinalis due to air trapping in the bowel wall that may rupture and cause benign pneumoperitoneum. Primary biliary cirrhosis may coexist with SSc.
Renal Involvement
Hypertension and chronic nonprogressive proteinuria are frequent in SSc. Scleroderma renal crisis, which is the most dreaded complication of SSc, occurs in 20-25% of patients, most commonly within 4 years of the onset of the disease. Until the advent of ACE inhibitor drugs, short-term survival of patients with scleroderma renal crisis was <10%.The pathogenesis of scleroderma renal crisis involves obliterative vasculopa-thy of the renal cortical arteries. Progressive reduction in renal blood flow, aggravated by vasospasm, leads to juxtaglomerular apparatus hyperplasia, renin secretion, and activation of the renin-angiotensin axis, with further renal vasoconstriction resulting in a vicious cycle that culminates in malignant hypertension. Factors that further compromise already impaired renal blood flow, such as dehydration and hypotension, play a role in precipitating scleroderma renal crisis. Risk factors include African-American race, male gender, diffuse and rapidly progressive skin involvement, and autoantibodies to RNA polymerase III. The presence of palpable tendon friction rubs, pericardial effusion, new unexplained anemia, and thrombocytopenia may predict impending scleroderma renal crisis. High-risk patients should be monitored closely and counseled to check their blood pressure daily. Patients with lcSSc only infrequently develop scleroderma renal crisis. Because there is a significant association between glucocorticoid use and the onset of scleroderma renal crisis, prednisone should be avoided in high-risk SSc patients.
Patients characteristically present with abrupt onset of malignant hypertension. They may complain of severe headache, blurred vision, and chest pain and have striking elevation of blood pressure. In approximately 10% of patients, blood pressure remains normal (normotensive renal crisis). Urinalysis shows proteinuria and microscopic hematuria; thrombocytopenia and evidence of a microangiopathic hemolysis with fragmented red blood cells is seen. Rapidly progressive oliguric renal failure generally follows. In some patients, scleroderma renal crisis is misdiagnosed as thrombotic thrombocytopenic purpura.A creatinine >3 mg/dL at presentation predicts poor outcome, with permanent hemodialysis and high mortality. Prompt aggressive intervention with ACE inhibitors to achieve blood pressure control before renal failure results in significantly improved prognosis.
Cardiac Involvement
Cardiac involvement is manifested by myocardial and pericardial disease and conduction system abnormalities. Cardiac involvement can also occur secondary to PAH and scleroderma renal crisis. Despite the presence of widespread obliterative vasculopathy in SSc, the frequency of clinical or pathological coronary artery disease is not elevated. Most patients with cardiac involvement remain asymptomatic until heart failure or serious arrhythmias occur. Overt signs of cardiac involvement in SSc are associated with increased mortality. Thallium perfusion studies document abnormal cardiac perfusion in a majority of patients. Raynaud’s-like episodic vasospasm of the coronary arteries has been described. Echocardiographic evidence of left ventricular diastolic dysfunction is frequent. Diastolic dysfunction may be due to hypertension or myocardial fibrosis, but its clinical significance is unclear. Myocarditis can develop in association with inflammatory polymyositis. Conduction defects and arrhythmias due to fibrosis or ischemia of the conduction system are frequent. Pericardial effusions may occur, causing symptoms and, rarely, tamponade.
Musculoskeletal Complications
Carpal tunnel syndrome occurs frequently and may be a presenting manifestation of SSc. Generalized arthralgia and stiffness are prominent in early disease.Joint mobility is progressively impaired, especially in patients with dcSSc. Most commonly affected are the hands, where contractures at the proximal interphalangeal joints and wrists develop, sometimes accompanied by tendon friction rubs characterized by leathery crepitation that can be heard or palpated upon passive movement. Tendon rubs are due to extensive fibrosis and adhesion of the tendon sheaths and fascial planes at the affected joint. Movement at the elbows, shoulders, and knees is frequently reduced. True joint inflammation is uncommon; however, occasional patients develop features of rheumatoid arthritis and, rarely, severe erosive asymmetrical polyarthritis of the joints in the hands. Muscle weakness may reflect deconditioning, disuse atrophy, and malnutrition. Less commonly, inflammatory myositis indistinguishable from idiopathic polymyositis may occur. A chronic noninflammatory myopathy characterized by atrophy and fibrosis in the absence of elevated muscle enzyme levels is seen in some patients with late-stage SSc. Bone resorption, a frequent late complication, occurs most commonly in the terminal phalanges, where it causes loss of the distal tufts (acro-osteolysis) (Fig. 7-5). Acro-osteolysis of the mandibular condyles can lead to bite difficulties. Osteolysis can also affect the ribs and distal clavicles.
Other Disease Manifestations
Many SSc patients develop dry eyes and dry mouth (sicca complex). Biopsy of the minor salivary glands shows fibrosis rather than focal lymphocytic infiltration characteristic ofprimary Sjögren’s syndrome (Chap. 8). Hypothyroidism is common and generally due to fibrosis of the thyroid gland. Whereas the central nervous system is generally spared in SSc, sensory trigeminal neuropathy due to fibrosis or vasculopathy can occur, presenting with gradual onset of pain and numbness. Pregnancy in women with SSc is associated with an increased rate of adverse fetal outcomes. Furthermore, worsening cardiopulmonary involvement may occur during pregnancy, and new onset of scleroderma renal crisis has been described. Erectile dysfunction is frequent in men with SSc and may be the initial disease manifestation. Inability to attain or maintain penile erection is due to vascular insufficiency and fibrosis.
Laboratory Features
Anemia is frequent in patients with SSc and may have different etiologies. Most common is a mild normocytic or microcytic anemia due to chronic inflammation. Serum iron is low or normal, whereas ferritin levels are elevated. Iron deficiency anemia may indicate gastrointestinal bleeding caused by watermelon stomach or chronic esophagitis. Macrocytic anemia, indicating a maturation disorder, may be caused by folate and vitamin B12 deficiency due to small bowel bacterial overgrowth and malabsorption, or by drugs that interfere with cellular DNA metabolism, such as methotrexate or alkylating agents. Acute microangiopathic hemolytic anemia, caused by mechanical trauma and fragmentation of red blood cells during their passage through microvessels coated with fibrin or platelet thrombi, frequently accompanies scleroderma renal crisis. Thrombocytopenia and leukopenia occur rarely and generally indicate drug toxicity. In contrast to other connective tissue diseases, the erythrocyte sedimentation rate (ESR) is generally normal; an elevation may indicate coexisting myositis or malignancy.
Antinuclear autoantibodies can be detected in almost all patients with SSc and are present at disease onset. Some of these autoantibodies, such as those directed against topoisomerase-I (Scl-70) and centromere, are very highly specific for SSc and are mutually exclusive. Furthermore, a patient’s specific autoantibody profile remains stable over time. Each of the eight distinct autoantibodies described in SSc shows a strong association with a particular disease phenotype (Table 7-4).Topoisomerase-I antibodies are detected in 31% of patients with dcSSc, but in only 13% of patients with lcSSc; conversely, anticentromere antibodies are detected in 38% of patients with lcSSc, but in only 2% of patients with dcSSc. Topoisomerase-I antibodies generally occur in patients with dcSSc and early-onset ILD. Anticentromere antibodies occur in patients with lcSSc with PAH, whereas cardiac and renal involvement and significant ILD are rare in these patients. Patients with topoisomerase-I antibody have reduced survival compared to those without this antibody; whereas patients with anticentromere antibody have improved survival compared to those without this antibody. The characteristic nucleolar immunofluorescence pattern of SSc detected on serological testing is due to antibody recognition of U3-RNP (fibrillarin), Th/To, and PM/Scl. No direct pathogenic role has been established for SSc-associated autoantibodies; however, recent studies indicate that antibody titers correlate with disease severity and fluctuate with disease activity.
Diagnosis
The diagnosis of SSc is made primarily on clinical grounds and is generally straightforward in patients with established disease. The presence of skin induration, with a characteristic symmetrical distribution pattern associated with typical visceral organ manifestations, establishes the diagnosis with a high degree of certainty. While the conditions listed in Table 7-1 may be associated with variable skin induration, the distribution pattern of these lesions, absence of Raynaud’s phenomenon, and lack of typical visceral organ manifestations or SSc-specific autoantibodies help to differentiate these conditions from SSc. Occasionally, full-thickness biopsy of the skin may be indicated to establish the diagnosis of scleredema, scleromyxedema, or nephrogenic systemic fibrosis. In lcSSc a history of antecedent Raynaud’s phenomenon and gastroesophageal reflux symptoms, coupled with the presence of sclerodactyly, often in combinations with telangiectasia and calcinosis cutis, helps to establish the diagnosis. The finding of digital tip pitting scars and radiological evidence of pulmonary fibrosis in the lower lobes are particularly helpful diagnostically. Primary Raynaud’s phenomenon is a common disorder that must be differentiated from early or limited SSc. Nailfold microscopy is particularly helpful in this situation, because in primary Raynaud’s phenomenon the nailfold capillaries are normal, whereas in SSc capillary abnormalities can be detected even before other disease manifestations.
Establishing the diagnosis of SSc in early disease may be a challenge. In patients with dcSSc, initial symptoms are often nonspecific and relate to inflammation. Raynaud’s phenomenon may be absent at this stage, and patients complain of fatigue, swelling, aching, and stiffness; muscle weakness and weight loss may be prominent. Physical examination may reveal diffuse edema and swelling of the fingers. Patients are sometimes diagnosed as having early rheumatoid arthritis, systemic lupus erythematosus, myositis, or, most commonly, undifferentiated connective tissue disease. Within weeks to months, Raynaud’s phenomenon develops, and the disease assumes its characteristic clinical features with advancing induration of the skin. The presence of antinuclear and SSc-specific autoantibodies, most commonly anticentromere or anti-topoisomerase-I, provides a high degree of diagnostic specificity. Raynaud’s phenomenon with fingertip ulcerations or other evidence of digital ischemia, coupled with telangiectasia, distal esophageal dysmotility, unexplained ILD, or PAH, or malignant hypertension with renal failure in the absence of skin induration, suggests the diagnosis of SSc sine scleroderma. These patients generally have anticentromere antibodies.
Treatment:
Systemic Sclerosis
OVERVIEW To date, no therapy has been shown to significantly alter the natural history of SSc. In contrast, multiple interventions are highly effective in alleviating the symptoms and in slowing the progression of the cumulative organ damage. A significant reduction in disease-related mortality has been noted during the past 25 years. Because of the marked heterogeneity in clinical presentations, patients with SSc need careful investigation, and evaluation and treatment approaches must be individually tailored according to each patient’s unique needs. Optimal management incorporates the following principles: prompt and accurate diagnosis; classification and risk stratification based on clinical and laboratory evaluation; early recognition of organ-based complications and assessment oftheir extent, severity,and likelihood of deterioration; ongoing regular monitoring for progression,disease activity,and response to therapy; and continuing patient education. In order to minimize irreversible organ damage,the approach to the management of life-threatening complications must be proac-tive,with regular screening and initiation of appropriate intervention at the earliest possible opportunity. In light of the highly complex and multisystemic nature of SSc, a holistic approach that integrates care by specialists from multiple disciplines is best. Most patients are treated with combinations of drugs that act upon different aspects of the disease. It is important that patients become familiar with the full spectrum of potential complications, have a thorough understanding of the therapeutic options and natural history of the disease, and be encouraged to partner with their physicians in its management.This typically requires a long-term relationship between patient and physician, with ongoing counseling and encouragement.
Disease-Modifying Treatments Immunosuppressive agents that are effective in controlling other connective tissue diseases have generally shown modest or no benefit in the treatment of SSc. Glucocorticoids may decrease stiffness and aching in patients with early-stage dcSSc but do not influence the progression of skin or internal organ involvement. Furthermore,use of glucocorticoids in high doses is associated with an increased risk of scleroderma renal crisis.Therefore,glucocorticoids should be avoided if possible;when absolutely necessary, they should be given at the lowest dose possible and for brief periods only. Cyclophosphamide has been extensively studied, in light of its efficacy in the treatment of vasculitis (Chap. 10), systemic lupus erythematosus (Chap. 4), and other autoimmune diseases (Chap. 3). A number of retrospective uncontrolled clinical trials evaluated the efficacy of daily oral and intermittent intravenous cyclophosphamide in SSc-related ILD. These studies, as well as a recent placebo-controlled multicenter clinical trial, showed that cyclophosphamide reduced the progression of ILD in patients with early symptomatic disease, with stabilization, and, rarely, modest improvement in abnormalities of pulmonary function and HRCT. Improvement in the extent of skin induration has also been noted. Patients with early-stage SSc and evidence of progressive pulmonary involvement appear to be candidates for cyclophosphamide therapy. Cyclophosphamide is generally given for 6-12 months, but the optimal duration of therapy has not been established.The benefits of cyclophosphamide need to be balanced by its potential toxicity. Well-recognized adverse effects include bone marrow suppression, opportunistic infections, hemorrhagic cystitis and bladder cancer, premature ovarian failure,and late secondary malignancies.
In small clinical trials, methotrexate, an antimetabolite used extensively in the treatment of rheumatoid arthritis, showed a modest therapeutic benefit. The potential profibrotic effects of methotrexate, manifested as infrequent liver cirrhosis and ILD, raise concern regarding its use in a fibrotic disorder. Mycophenolate mofetil treatment was associated with improved skin induration in uncontrolled studies and was generally well tolerated. Therapeutic immunomodulation using cyclosporine, azathioprine, extracorporeal photophore-sis,thalidomide,or rapamycin is currently not well supported by the literature. Immune ablation using highdose chemotherapy,followed by autologous peripheral stem cell reconstitution, has been performed in SSc. Because uncontrolled studies have shown that stem cell transplantation in patients with extensive SSc and poor prognosis was associated with variable clinical response, this form of intervention is currently undergoing evaluation in randomized prospective clinical trials. In light of its substantial morbidity and mortality,autologous stem cell transplantation in SSc is still considered experimental.
Because widespread tissue fibrosis causes progressive organ damage in dcSSc, drugs that interfere with the fibrotic process represent a rational approach to therapy. D-penicillamine has been extensively used in SSc as an antifibrotic agent. Retrospective studies indicated that, by virtue of its immunosuppressive activity and ability to prevent cross-linking of extracellular collagen fibers, D-penicillamine stabilized and improved skin induration, prevented new internal organ involvement, and improved survival. However, a randomized, controlled clinical trial in early active SSc found no difference in the extent of skin involvement between patients treated with standard-dose (750 mg/d) or very low-dose (125 mg every other day) D-penicillamine. A randomized clinical trial found that recombinant human relaxin was not significantly better than placebo in improving the total skin score or pulmonary function or in reducing functional disability in patients with SSc and was associated with serious renal adverse events, the majority of which occurred after stopping the infusion. Minocycline and INF-γ have failed to show meaningful clinical benefit in small studies.
The goal of vascular therapy is to control episodes of Raynaud’s phenomenon, prevent the development and enhance the healing of ischemic complications,and slow the progression of obliterative vasculopathy. Patients with Raynaud’s phenomenon should be instructed to dress warmly, minimize cold exposure or stress,and avoid drugs that could precipitate or exacerbate vasospastic episodes. Some patients may respond to biofeedback therapy.Calcium channel blockers such as nifedepine or diltiazem are commonly used but show only moderate benefit, and their use is often limited by side effects (palpitations,dependent edema,light-headedness).While ACE inhibitors are not effective for reducing the frequency or severity of episodes, angiotensin II receptor blockers such as losartan are effective and generally well tolerated. Additional vasoactive therapies for Raynaud’s phenomenon include a1-adrenergic receptor blockers (e.g., prazosine), 5-phosphodiesterase inhibitors (e.g., sildenafil),serotonin reuptake inhibitors (e.g.,fluoxetine), topical nitroglycerine, and intravenous prostaglandins. Low-dose aspirin and dipyridamole prevent platelet aggregation and may have a role as adjunctive agents. In patients with ischemic ulcerations on the fingers, the endothelin-1 receptor antagonist bosentan reduces the development of new ulcers. Digital sympathectomy may be effective in some patients with severe Raynaud’s phenomenon associated with ischemia. Empiric longterm therapy with statins and antioxidants may delay the progression of vascular damage and obliteration.
Treatment of Gastrointestinal Complications Because gastroesophageal reflux is very common, all patients with SSc should be treated for this complication. Significant reflux may occur in the absence of symptoms. Patients should be instructed to elevate the head of the bed and eat frequent small meals. Proton pump inhibitors and H2 blockers are effective and may need to be given in relatively high doses. Recurrent bleeding from vascular ectasia in the gastric antrum (watermelon stomach) is amenable to treatment with laser photocoagulation. Bacterial overgrowth due to small-bowel dysmotility causes bloating and diarrhea and may lead to malabsorption and severe malnutrition. Aggressive treatment with short courses of rotating broad-spectrum antibiotics such as metronida-zole,erythromycin,and tetracycline can eradicate bacterial overgrowth. Parenteral hyperalimentation is indicated if malnutrition develops. Chronic hypomotility of the small bowel may respond to octreotide injections.
Treatment of Pulmonary Arterial Hypertension Patients with SSc should be screened for the presence of PAH on a regular basis.When PAH is symptomatic, treatment should be started with an oral endothelin-1 receptor antagonist. Most patients should also receive diuretics, oral anticoagulation, and digoxin when appropriate. Endothelin-1 receptor antagonists such as bosentan have been shown to improve exercise tolerance and slow the rate of clinical deterioration in pulmonary arterial hypertension. If hypoxemia is documented, supplemental oxygen should be given by nasal cannula in order to avoid hypoxia-induced secondary pulmonary vasoconstriction. Inhibitors of phosphodiesterase type 5 (e.g., sildenafil) have been shown to have short-term efficacy in PAH and may be used in combination with bosentan. If inadequate clinical response or progression of disease is seen, parenteral prostacyclin analogues may be used. Epoprostenol or treprostinil are administered intravenously or by continuous subcutaneous infusion, and iloprost by frequent inhalations. Lung transplantation remains an option for some SSc patients who fail therapy.
Treatment of Renal Crisis Scleroderma renal crisis is a medical emergency because its outcome is largely determined by the extent of renal damage present at the time when aggressive therapy is initiated. Prompt recognition of impending or early scleroderma renal crisis is therefore essential, and efforts should be made to avoid its occurrence. High-risk patients with early SSc and extensive and progressive skin involvement should be instructed to monitor their blood pressure daily and report significant alterations to their physician immediately. They should avoid nonsteroidal anti-inflammatory drugs (NSAIDs) and glucocorticoids. When scleroderma renal crisis occurs, treatment should be started promptly with ACE inhibitors. Kidney biopsy is rarely indicated in this setting.Short-term dialysis may be appropriate, particularly because substantial renal recovery can occur following renal crisis, and patients may be able to discontinue dialysis. Kidney transplantation is considered for patients who are unable to discontinue dialysis after 1-2 years.
Skin Care Because skin involvement in SSc is never life threatening,stabilizes,and may even regress spontaneously over time, the overall management of the disease should not be dictated by its cutaneous manifestations. The inflammatory symptoms of early skin involvement can be effectively controlled with systemic antihistamines and cautious use of low-dose glucocorticoids (less than 5 mg/d of prednisone) for brief periods. Retrospective studies have shown that D-penicillamine reduced the extent and progression of skin induration; however,these benefits could not be substantiated in a controlled prospective trial. Cyclophosphamide and methotrexate have also been shown to have modest effects on skin induration. Because induration is associated with dryness, patients should use hydrophilic ointments and bath oils. Regular skin massage is helpful. Telangiectasia may present a cosmetic problem, especially when they occur on the face. Treatment with pulsed dye laser may be effective. Fingertip ulcerations should be protected by occlusive dressing to promote healing and prevent infection. Infected skin ulcers are treated with topical antibiotics. Surgical débridement may be indicated. No therapy has been shown to be effective in preventing the formation of calcific soft tissue deposits or in promoting their dissolution.
Course and Prognosis
The natural history of SSc is highly variable and difficult to predict, especially in early stages when the specific disease subset—diffuse or limited cutaneous form—is not clear. Patients with dcSSc have a more rapidly progressive disease and worse prognosis than those with lcSSc.
In dcSSc, early inflammatory symptoms such as fatigue, edema, arthralgia, and pruritus tend to subside 2-4 years after the onset of disease, and the extent of skin thickening reaches a plateau after which it generally shows slow regression. It is during the early edematous stage, generally lasting <3 years, that visceral organ involvement develops and progresses. While existing visceral organ involvement, such as pulmonary fibrosis, may continue to progress, new organ involvement is rare after the skin involvement reaches its peak. Scleroderma renal crisis almost invariably occurs within the first 4 years of disease. In dcSSc patients with late-stage disease (>6 years), the skin is usually soft and atrophic. Skin regression characteristically occurs in an order that is the reverse of initial involvement, with softening on the trunks followed by proximal and then distal extremities. Sclerodactyly and finger contractures generally persist. Cutaneous telangiectasia and calcinosis are common, making it difficult to differentiate late-stage dcSSc from lcSSc. Relapse or recurrence of skin thickening after the peak of skin involvement has been reached is rare. Patients with lcSSc follow a clinical course that is markedly different than that of dcSSc, and lcSSc carries a better prognosis. In this subset of SSc, Raynaud’s phenomenon typically precedes other disease manifestations by years or even decades. Visceral organ complications such as PAH generally develop late and tend to be slowly progressive.
SSc confers a substantial increase in the risk of premature death, with five- to eightfold higher age- and gender-adjusted mortality rates compared to the general population. In one population-based study of SSc patients with all forms of the disease, the median survival was 11 years. In patients with dcSSc, 5- and 10-year survivals are 70 and 55%, respectively, whereas in patients with lcSSc, 5- and 10-year survivals are 90 and 75%, respectively. The prognosis of SSc correlates with the extent of skin involvement, which itself is a surrogate for visceral organ involvement. Major causes of death in SSc are PAH, pulmonary fibrosis, gastrointestinal involvement, cardiac involvement, and scleroderma renal crisis. Lung cancer and excess cardiovascular deaths also contribute to increased mortality. Markers of worse prognosis include male gender, older age of disease onset, African-American race, extensive skin thickening with truncal involvement, evidence of significant or progressive visceral organ involvement, and the presence of topoisomerase-I antibodies. Additional findings demonstrable at initial evaluation that are associated with increased mortality include an elevated ESR, anemia, and proteinuria. In one study, SSc patients with extensive skin involvement, lung vital capacity <55% predicted, significant gastrointestinal involvement (pseudoobstruction or malabsorption), evidence of cardiac involvement (arrhythmias or congestive heart failure), or scleroderma renal crisis had a cumulative 9-year survival <40%.The severity of PAH is itself strongly associated with mortality, and SSc patients who had a mean pulmonary arterial pressure >45 mmHg had a 33% 3-year survival.The introduction of ACE inhibitors in the early 1980s had a dramatic impact on survival of patients with scleroderma renal crisis, from a <20% 1-year survival in the pretreatment era to a >70% 1-year survival currently
Mixed Connective Tissue Disease
Patients with features of lcSSc coexisting with features of systemic lupus erythematosus, polymyositis, and rheumatoid arthritis may have mixed connective tissue disease (MCTD). This overlap syndrome is generally associated with the presence of high titers of autoantibodies to U1-RNP. The characteristic initial presentation is Raynaud’s phenomenon associated with puffy fingers and myalgia. Gradually, lcSSc features of sclerodactyly, calcinosis, and cutaneous telangiectasia develop. Skin rashes suggestive of systemic lupus erythematosus (malar rash, photosensitivity) or of dermatomyositis (heliotrope rash on the eyelids, erythematous rash on the knuckles) occur. While arthralgia is common, some patients develop erosive polyarthritis. Pulmonary fibrosis and isolated or secondary PAH may develop. Other manifestations include esophageal dysmotility, pericarditis, Sjögren’s syndrome, and renal disease, especially membranous glomerulonephritis. Laboratory evaluation indicates features of inflammation with elevated ESR and hypergammaglob-ulinemia.While anti-U1RNP antibodies are detected in the serum in high titers, SSc-specific autoantibodies are not found. In contrast to SSc, patients with MCTD often show a good response to treatment with glucocorticoids, and the long-term prognosis is better than that of SSc. Whether MCTD is a truly distinct entity or is, rather, a subset of systemic lupus erythematosus or SSc remains controversial.
Eosinophilic Fasciitis
Eosinophilic fasciitis is a rare idiopathic disorder associated with scleroderma-like induration of the skin that generally develops rapidly and involves the upper extremities. Adults are primarily affected. The skin has a coarse cobblestone “peau d’orange” appearance. In contrast to SSc, internal organ involvement is rare in eosinophilic fasciitis, and Raynaud’s phenomenon is absent. Furthermore, skin involvement spares the fingers. Full-thickness biopsy of the lesional skin reveals marked subcutaneous fibrosis and thickening of the subcutaneous fascial layers. Inflammation and eosinophil infiltration in the fascia are variably present. In the acute phase of the illness, peripheral blood eosinophilia is generally present but may be transient. Autoantibodies do not occur. Treatment with glucocorticoids leads to prompt resolution of the eosinophilia, but skin changes show only slow and variable improvement. The prognosis of patients with eosinophilic fasciitis is good.