Relapsing polychondritis is an uncommon inflammatory disorder of unknown cause characterized by an episodic and generally progressive course affecting predominantly the cartilage of the ears, nose, and laryngotracheo-bronchial tree. Other manifestations include scleritis, neu-rosensory hearing loss, polyarthritis, cardiac abnormalities, skin lesions, and glomerulonephritis. The peak age of onset is between 40 and 50 years, but relapsing polychondritis may affect children and the elderly. It is found in all races, and both sexes are equally affected. No familial tendency is apparent. A significantly higher frequency of HLA-DR4 has been found in patients with relapsing polychondritis than in normal individuals. A predominant subtype allele(s) of HLA-DR4 was not found. Approximately 30% of patients with relapsing polychondritis will have another rheumatologic disorder, the most frequent being systemic vasculitis, followed by rheumatoid arthritis, systemic lupus erythematosus (SLE), Sjögren’s syndrome, or ankylosing spondylitis. Nonrheumatic disorders associated with relapsing polychondritis include inflammatory bowel disease, primary biliary cirrhosis, and myelodysplastic syndrome (Table 12-1).
Diagnostic criteria were suggested over 20 years ago by McAdam et al. and modified by Damiani and Levine a few years later. These criteria continue to be generally used in clinical practice. McAdam et al. proposed the following: (1) recurrent chondritis of both auricles; (2) nonerosive inflammatory arthritis; (3) chondritis of nasal cartilage; (4) inflammation of ocular structures, including conjunctivitis, keratitis, scleritis/episcleritis, and/or uveitis; (5) chondritis of the laryngeal and/or tracheal cartilages; and (6) cochlear and/or vestibular damage manifested by neurosensory hearing loss, tinnitus, and/or vertigo. The diagnosis is certain when three or more of these features are present along with a positive biopsy from the ear, nasal, or respiratory cartilage. Damiani and Levine later suggested that the diagnosis could be made when one or more of the above features and a positive biopsy were present, when two or more separate sites of cartilage inflammation were present that responded to glucocorticoids or dapsone, or when three or more of the above features were present. A biopsy is not necessary in most patients with clinically evident disease.
Pathology and Pathophysiology
The earliest abnormality of hyaline and elastic cartilage noted histologically is a focal or diffuse loss of basophilic staining indicating depletion of proteoglycan from the cartilage matrix. Inflammatory infiltrates are found adjacent to involved cartilage and consist predominantly of mononuclear cells and occasional plasma cells. In acute disease, polymorphonuclear white cells may also be present. Destruction of cartilage begins at the outer edges and advances centrally. There is lacunar breakdown and loss of chondrocytes. Degenerating cartilage is replaced by granulation tissue and later by fibrosis and focal areas of calcification. Small loci of cartilage regeneration may be present.
| TABLE 12-1 |
|
Systemic vasculitis |
|
Rheumatoid arthritis |
|
Systemic lupus erythematosus |
|
Sjögren’s syndrome |
|
Spondyloarthritides |
|
Behget’s syndrome |
|
Inflammatory bowel disease |
|
Primary biliary cirrhosis |
|
Myelodysplastic syndrome |
aSystemic vasculitis is the most common association followed by rheumatoid arthritis, systemic lupus erythematosus, and Sjögren’s syndrome.
Immunofluorescence studies have shown immunoglobulins and complement at sites of involvement. Extracellular granular material observed in the degenerating cartilage matrix by electron microscopy has been interpreted to be enzymes, immunoglobulins, or proteoglycans.
Immunologic mechanisms play a role in the pathogenesis of relapsing polychondritis. Immunoglobulin and complement deposits are found at sites of inflammation. In addition, antibodies to type II collagen and to matrilin-1 and immune complexes are detected in the sera of some patients. The possibility that an immune response to type II collagen may be important in the pathogenesis is supported experimentally by the occurrence of auricular chondritis in rats immunized with type II collagen. Antibodies to type II collagen are found in the sera of these animals, and immune deposits are detected at sites of ear inflammation. Humoral immune responses to type IX and type XI collagen, matrilin-1, and cartilage oligomeric matrix protein have been demonstrated in some patients. In a study, rats immunized with matrilin-1 were found to develop severe inspiratory stridor and swelling of the nasal septum. The rats had severe inflammation with erosions of the involved cartilage, which was characterized by increased numbers of CD4+ and CD8+ T cells in the lesions. The cartilage of the joints and ear pinna was not involved.All had IgG antibodies to matrilin-1. Matrilin-1 is a noncollagenous protein present in the extracellular matrix in cartilage. It is present in high concentrations in the trachea and is also present in the nasal septum but not in articular cartilage. A subsequent study demonstrated serum anti-matrilin-1 antibodies in approximately 13% of patients with relapsing polychondritis; approximately 70% of these patients had respiratory symptoms. Cell-mediated immunity may also be operative in causing tissue injury, since lymphocyte transformation can be demonstrated when lymphocytes of patients are exposed to cartilage extracts. T cells specific for type II collagen have been found in some patients, and CD4+ T cells have been observed at sites of cartilage inflammation. The accumulating data strongly suggest that both humoral and cell-mediated immunity play an important role in the pathogenesis of relapsing polychondritis.
Dissolution of cartilage matrix can be induced by the intravenous injection of crude papain, a proteolytic enzyme, into young rabbits, which results in collapse of their normally rigid ears within 4 h. Reconstitution of the matrix occurs in about 7 days. In relapsing polychondritis, loss of cartilage matrix also most likely results from action of proteolytic enzymes released from chondrocytes, polymorphonuclear white cells, and monocytes that have been activated by inflammatory mediators.
Clinical Manifestations
The onset of relapsing polychondritis is frequently abrupt with the appearance of one or two sites of cartilaginous inflammation. Fever, fatigue, and weight loss occur and may precede the clinical signs of relapsing polychondritis by several weeks. Relapsing polychondritis may go unrecognized for several months or even years in patients who only initially manifest intermittent joint pain and/or swelling, or who have unexplained eye inflammation, hearing loss, valvular heart disease, or pulmonary symptoms. The pattern of cartilaginous involvement and the frequency of episodes vary widely among patients.
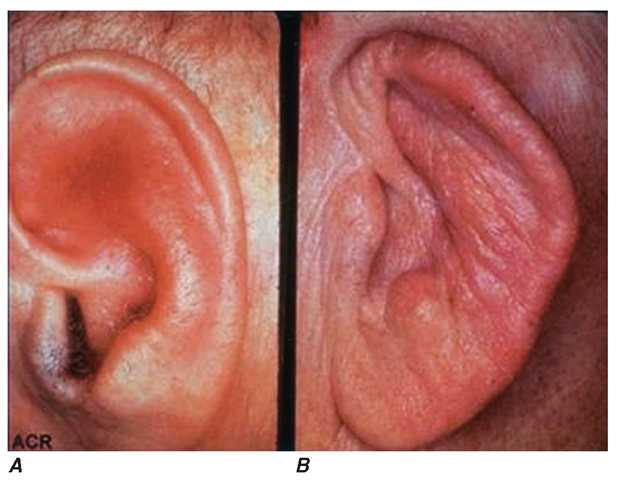
Auricular chondritis is the most frequent presenting manifestation of relapsing polychondritis in 40% of patients and eventually affects about 85% of patients (Table 12-2). One or both ears are involved, either sequentially or simultaneously. Patients experience the sudden onset of pain, tenderness, and swelling of the cartilaginous portion of the ear (Fig. 12-1).
TABLE 12-2
CLINICAL MANIFESTATIONS OF RELAPSING POLYCHONDRITIS
|
FREQUENCY, % |
||
|
CLINICAL FEATURE |
PRESENTING |
CUMULATIVE |
|
Auricular chondritis |
43 |
89 |
|
Arthritis |
32 |
72 |
|
Nasal chondritis |
21 |
61 |
|
Ocular inflammation |
18 |
59 |
|
Laryngotracheal symptoms |
23 |
55 |
|
Reduced hearing |
7 |
40 |
|
Saddle nose deformity |
11 |
25 |
|
Cutaneous |
4 |
25 |
|
Laryngotracheal stricture |
15 |
23 |
|
Vasculitis |
2 |
14 |
|
Elevated creatinine |
7 |
13 |
|
Aortic or mitral regurgitation |
0 |
12 |
FIGURE 12-1
A. The pinna is erythematous, swollen, and tender. Not shown is the ear lobule that is spared as there is no underlying cartilage. B. The pinna is thickened and deformed. The destruction of the underlying cartilage results in a floppy ear.
Earlobes are spared because they do not contain cartilage. The overlying skin has a beefy red or violaceous color. Prolonged or recurrent episodes result in a flabby or droopy ear as a sequela of cartilage destruction. Swelling may close off the eustachian tube (causing otitis media) or the external auditory meatus, either of which can impair hearing. Inflammation of the internal auditory artery or its cochlear branch produces hearing loss, vertigo, ataxia, nausea, and vomiting.Vertigo is almost always accompanied by hearing loss. The cartilage of the nose becomes inflamed during the first or subsequent attacks. Approximately 50% of patients will eventually have nose involvement. Patients may experience nasal stuffiness, rhinorrhea, and epistaxis. The bridge of the nose becomes red, swollen, and tender and may collapse, producing a saddle deformity (Fig. 12-2). In some patients, the saddle deformity develops insidiously without overt inflammation. Saddle nose is observed more frequently in younger patients, especially in women.
Arthritis is the presenting manifestation in relapsing polychondritis in approximately one-third of patients and may be present for several months before other features appear. Eventually, more than half the patients will have arthritis. The arthritis is usually asymmetric and oligo- or polyarticular, and it involves both large and small peripheral joints. An episode of arthritis lasts from a few days to several weeks and resolves spontaneously without residual joint deformity.Attacks of arthritis may not be temporally related to other manifestations of relapsing polychondritis. The joints are warm, tender, and swollen. Joint fluid has been reported to be noninflammatory. In addition to peripheral joints, inflammation may involve the costochondral, sternomanubrial, and sternoclavicular cartilages. Destruction of these cartilages may result in a pectus excavatum deformity or even a flail anterior chest wall. Relapsing polychondritis may occur in patients with preexisting rheumatoid arthritis, Reiter’s syndrome, psoriatic arthritis, or ankylosing spondylitis.
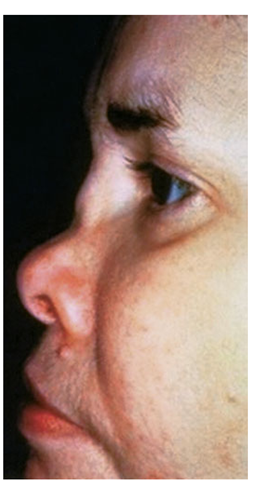
FIGURE 12-2
Saddle nose results from destruction and collapse of the nasal cartilage.
Eye manifestations occur in more than half of patients and include conjunctivitis, episcleritis, scleritis, iritis, and keratitis. Eye involvement is seldom the presenting feature. Ulceration and perforation of the cornea may occur and cause blindness. Other manifestations include eyelid and periorbital edema, proptosis, cataracts, optic neuritis, extraocular muscle palsies, retinal vasculitis, and renal vein occlusion.
Laryngotracheobronchial involvement occurs in ~50% of patients. Symptoms include hoarseness, a nonproductive cough, and tenderness over the larynx and proximal trachea. Mucosal edema, strictures, and/or collapse of laryngeal or tracheal cartilage may cause stridor and life-threatening airway obstruction necessitating tracheostomy. Collapse of cartilage in bronchi leads to pneumonia and, when extensive, to respiratory insufficiency
Aortic regurgitation occurs in about 5% of patients and is due to progressive dilation of the aortic ring or to destruction of the valve cusps. Mitral and other heart valves are affected less often. Other cardiac manifestations include pericarditis, myocarditis, and conduction abnormalities. Aneurysms of the proximal, thoracic, or abdominal aorta may occur even in the absence of active chondritis and occasionally rupture.
Systemic vasculitis may occur in association with relapsing polychondritis. Vasculitides include isolated cutaneous vasculitis, polyarteritis nodosa, giant cell arteritis, and Takayasu’s arteritis (Chap. 10). Neurologic abnormalities usually occur as a result of underlying vasculitis, manifesting as seizures, strokes, ataxia, and peripheral and cranial nerve neuropathies. Cranial nerves II, III,VI, and VII are most often involved.Approximately 25% of patients have skin lesions, none of which is characteristic for relapsing polychondritis but can reflect an associated vasculitis. These include purpura, erythema nodosum, erythema multiforme, angioedema/urticaria, livedo reticularis, and panniculitis. Segmental necrotizing glomerulonephritis with crescent formation has been noted in some patients, usually in association with microscopic polyangiitis, but may occur in the absence of systemic vasculitis.
The course of disease is highly variable, with episodes lasting from a few days to several weeks and then subsiding spontaneously. Attacks may recur at intervals varying from weeks to months. In other patients, the disease has a chronic, smoldering course. In a few patients, the disease may be limited to one or two episodes of cartilage inflammation. In one study, the 5-year estimated survival rate was 74% and the 10-year survival rate 55%. In contrast to earlier series, only about half the deaths could be attributed to relapsing polychondritis or complications of treatment. Pulmonary complications accounted for only 10% of all fatalities. In general, patients with more widespread disease have a worse prognosis.
Laboratory Findings
Mild leukocytosis and normocytic, normochromic anemia are often present. Eosinophilia is observed in 10% of patients. The erythrocyte sedimentation rate and C-reactive protein are usually elevated. Rheumatoid factor and antinuclear antibody tests are occasionally positive in low titers. Antibodies to type II collagen are present in fewer than half the patients and are not specific. Circulating immune complexes may be detected, especially in patients with early active disease. Elevated levels of γ globulin may be present. Antineutrophil cytoplasmic antibodies (ANCA), either cytoplasmic (cANCA) or perinuclear (pANCA), are found in some patients with active disease. The upper and lower airways can be evaluated by imaging techniques such as linear tomography, laryngotracheography, and CT, and by bronchoscopy. MRI is helpful in evaluation of the larynx and trachea. Bronchography is performed to demonstrate bronchial narrowing. Intrathoracic airway obstruction can also be evaluated by inspiratory-expiratory flow studies. The chest film may show narrowing of the trachea and/or the main bronchi, widening of the ascending or descending aorta due to an aneurysm, and cardiomegaly when aortic insufficiency is present. MRI can be used in assessing aortic aneurysmal dilatation. Radiographs may show calcification at previous sites of cartilage damage involving ear, nose, larynx, or trachea.
Diagnosis
Diagnosis is based on recognition of the typical clinical features. Biopsies of the involved cartilage from the ear, nose, or respiratory tract will confirm the diagnosis but are only necessary when clinical features are not typical. Patients with Wegener’s granulomatosis may have a saddle nose and pulmonary involvement but can be distinguished by the absence of auricular involvement and the presence of granulomatous lesions in the tracheobronchial tree. Patients with Cogan’s syndrome have interstitial keratitis and vestibular and auditory abnormalities, but this syndrome does not involve the respiratory tract or ears. Reiter’s syndrome may initially resemble relapsing polychondritis because of oligoarticular arthritis and eye involvement, but it is distinguished in time by the appearance of urethritis and typical mucocutaneous lesions and the absence of nose or ear cartilage involvement. Rheumatoid arthritis may initially suggest relapsing polychondritis because of arthritis and eye inflammation. The arthritis in rheumatoid arthritis, however, is erosive and symmetric. In addition, rheumatoid factor titers are usually high compared with those in relapsing polychondritis. Bacterial infection of the pinna may be mistaken for relapsing polychondritis but differs by usually involving only one ear, including the earlobe. Auricular cartilage may also be damaged by trauma or frostbite.
Relapsing polychondritis may develop in patients with a variety of autoimmune disorders, including SLE, rheumatoid arthritis, Sjögren’s syndrome, and vasculitis. In most cases, these disorders antedate the appearance of polychondritis, usually by months or years. It is likely that these patients have an immunologic abnormality that predisposes them to development of this group of autoimmune disorders.
Treatment:
Relapsing Polychondritis
In patients with active chondritis,prednisone,40-60 mg/d, is often effective in suppressing disease activity; it is tapered gradually once disease is controlled. In some patients, prednisone can be stopped, while in others low doses in the range of 10-15 mg/d are required for continued suppression of disease. Dapsone instead of prednisone has been effective in suppressing inflammation in some patients. Immunosuppressive drugs such as methotrexate,cyclophosphamide,azathioprine, or cyclosporine should be reserved for patients who fail to respond to prednisone or who require high doses for control of disease activity. Patients with significant ocular inflammation often require intraocular steroids as well as high doses of prednisone. A small retrospective series of nine patients did not find anti-CD20 (rituximab) to provide benefit, although this experience remains too small to draw firm conclusions. Heart valve replacement or repair of an aortic aneurysm may be necessary. When obstruction is severe, tracheostomy is required. Stents may be necessary in patients with tracheobronchial collapse.