Introduction
Low Back Pain (LBP) is a common musculoskeletal disorder causing huge humanitarian and economical costs (Andersson, 1999). It is often classified, according to duration of pain, as acute (short term), sub-acute (intermediate) and chronic (long-term) and is typically referred to as being specific or non-specific (Andersson, 1999; Merskey and Bogduk, 1994). Specific LBP refers to symptoms caused by ‘red flags’ such as spinal fractures, cancers, infections, and cauda equina syndrome. However, approximately 90% of cases of back pain have no identifiable cause and are designated as non-specific (Deyo and Weinstein, 2001).
Non-specific LBP is described as a "mechanical" back pain of musculoskeletal origin in which symptoms vary with physical activity. Previouse studies have linked it’s origin to various sources as follows: Matthews and Yates (1962) had demonstrated, with the help of epidurography, the presence of disc hernia which was resolved following mobilization; Irritation of spinal nerves causes spinal segmental sensitization, which limits the dynamic range of spinal segment mobility (Naguszewski et al, 2001; Cassius et al, 2002); unguided movement at the spine may strain the interspinous ligament to irritate the spinal segment (Lamb 1979; Cassius et al, 2002). Similarly, disc injury or gradually progressive micro trauma ends up in motion segment fusion which facilitates the deposition of collagen, hypo-mobility and pain (Lamb, 1979; Gose et al, 1998). Also, degenerative changes place the sclerotome, autonomic, motor and sensory systems in a hyper-excitable state, increases blood vessel tone, thus facilitating the release of endogenous algesic chemicals that irritate nociceptors (Lamb, 1979; Shacklock, 1995; Egwu et al, 2003). In addition, degeneration of the disc leads to a loss in disc height, thus reducing interpedicular distance, neural foraminal vertical height which may become stenotic (Matthews and Yates, 1962; Naguszewski et al, 2001). Facet changes and end-plate degeneration lead to osteophytes and leaping, which may encroach on the neural foramina anteriorly and/or posterior (Naguszewski et al, 2001). All of these eventuate into irritant focus, dysfunction and distorted neuro-dynamics with ectopic discharge that are the problems challenging the back pain patient. (Naguszewski et al, 2001; Amir et al, 1997; Amir et al, 1999; Devor, 1999). Moreso, physiological evidence shows that ectopic discharge of noxious impulses from nerve irritation sustains pain by triggering or enhancing sinusoidal voltage oscillation in dorsal root ganglion membrane potential (Amir et al, 1997; Amir et al,1999; Devor, 1999).
However, current reports suggest that the varieties of response to a painful experience are shaped by culture, literacy level and socio-economic status and are associated with the feelings of suffering, distress, functional disability, depression and so on (Merskey and Bogduk, 1994; Andersson, 1999). For instance Green et al (2003) observed that Caucasians report their pain promptly while African Americans with chronic pain report pain late and have more pain, depression, post traumatic stress disorders and impairment in their physical, emotional and social health. The above findings suggest that mood and other psycho-social states such as functional disability and depression may be crucial factors in determining who complains of LBP and their psycho-social response to it.
Depression (Dn) is a psychosocial condition characterized by difficulty in sleeping and concentration, decreased appetite and libido for at least 14 days. Other symptoms of depression are loss of interest and enjoyment, reduced energy, being easily fatigued, diminished activity, marked tiredness on slight effort, reduced concentration and attention on a task, reduced confidence and self-esteem, feeling of guilt and unworthiness, bleak and pessimistic views of the future and ideas or acts of self-destruction or suicide (WHO, 2001; Worz, 2003). On the other hand, Functional Disability (FD) is impairment in performing age-appropriate physical, mental, and social activities in daily life. It could be caused by pain, physical, cognitive and other mental impairments (Anthony and Schanberg, 2003). Non specific LBP is known to have a relationship with Dn and FD; however, the influence of duration and intensity of LBP on levels of Dn and FD is not clearly understood (Dworkin and Gitlin, 1991; Croft et al., 1995; Fishbain et al, 1997).
In addition, the term ‘depression’ is a continuum that includes lower mood states lacking clinical significance. However, at the other extreme of the continuum includes major (clinical) depressive disorders requiring clinical attention. Major Depression (MDn) is a mental disorder characterized by an all encompassing low mood, accompanied by low self -esteem and by loss of interest or pleasure in normally enjoyable activities (American Psychiatric Association, 1994). It is known that patients with MDn often do not comply with prescribed treatment regime, and if not detected in time worsen the person’s physical health and slow down recovery from other ailments (American Psychiatric Association, 1994; Worz, 2003).
The prevalence rate of MDn has been reported in developed countries (Sullivan et al., 1992; Banks and Kerns, 1996; Hope and Foreshaw, 1999; Caragee, 2001), however, information concerning the prevalence of MDn among Nigerian patients with Chronic LBP (CLBP) is scant. It is important to know the rate occurrence of MDn among Nigerian patients as it will help clinicians to look out for red flags indicating the presence of MDn to facilitate decision on which LBP patient will need psychoanalysis and therapy to enhance compliance and/or efficacy of chemotherapy or physiotherapy for LBP. This study therefore examined the relationship of CLBP duration and intensity with, Dn and FD and also estimated the prevalence rate of MDn among Nigerian patients with CLBP.
Method
Subjects: one hundred patients (41 male, 59 female) with chronic non specific LBP (aged range 20 to 85 years, mean age 54±12.84years) participated in this study. These were patients with LBP of not less than 3 months duration seen in the Physiotherapy Departments of Obafemi Awolowo University Teaching Hospitals Complex (OAUTHC), Ile-Ife; Ladoke Akintola University Teaching Hospital,Osogbo; Osun State Hospital,Asubiaro and Ilesa units and National Orthopaedic Hospital,Igbobi, Lagos all in south west Nigeria between February 5 and September 19, 2010. Prior to this, ethical clearance was obtained from the Ethics and Research Committee of OAUTHC, permission was sort and obtained from the head of Physiotherapy Department of each participating hospital and informed consent was obtained from the patient after explaining the research procedure.
In oder to ensure particpation of indigenouse Yoruba speaking patients, Beck Depression Inventory II and Oswestry Disability Index 2.0 were translated into Yoruba language at the Department of Linguistics and African language, Obafemi Awolowo University, Ile-Ife, Nigeria. Similarly, to ensure validity of the translated questionnaires, ten patients with nonspecific low back pain low back pain who were literate in both English and Yoruba language were requested to respond to the English version of the questionnaires and after ten minutes, they were also requested to respond to the translated one without prior knowledge that they would be filling the Yoruba translation. The translated questionnaires were found to be valid as all of them chose the same options in each of the questionnaires.
Inclution criteria:
1. Clinical diagnosis of LBP by a physician,
2. Pain duration not less than three months
3. Absence of any other ailment such as headache, infection, fever etc that have pain as one of its symptoms,
4. No history of mental illness,
5. No physical disability,
6. No history of recent life stressing events such as bereavement, huge financial loss or job loss,
7. literacy in either Yoruba or English language
Procedure: On arriving into the consulting room, patient’s height was measured using a validated height metre. The subjects stood erect, barefoot on a flat surface, with the occiput, upper back, buttocks and heels, touching the height metre. In line with the view of Steele & Spurgeon (1983), the upper margin of the external auditory canal opening were in the Frankfurt horizontal plane, the point of greatest height to the nearest 0.1cm was then marked off on the height metre. Weight was measured to the nearest 0.1Kg with a weighing scale (Hanson Company, Ireland) and Body Mass Index (BMI) was later calculated by dividing the respondent’s weight by the square of his or her height (Egwu et al, 2007). All measurements were taken by the same examiner with subjects on minimum clothing. Semantic differential scale (Olaogun et al, 2004) which has both English and Yoruba versions was giving to the subject to respond to alongside the above questionnaires. The subjects were then requested to choose and respond to either the English or the Yoruba version of the questionnaires and rate their pain accordingly.
Data analysis
Descriptive statistics of percentage, mean and standard deviation were used to summarize the subjects’ age, height, weight, BMI, pain duration, pain intensity, Dn and FD scores. Spearman rank order correlation coefficient and Chi-square test were used to assess relationships and differences respectively, among the variables. Data were analyzed using Statistical Package for Social Sciences (SPSS) software version16. Significance was fixed at an alpha level of 0.05.
Results
The minimum, maximum, range, mean and standard deviation of the physical characteristics (age, weight, height, BMI), duration and intensity of pain, Dn and FD scores of the patients are shown in table 1. It can be seen from this table that on the average, subjects were 54 years old weighing 74 kilogram with BMI of 28 Kg/m2. their pain had lasted for an average of 26 months with an intensity of 6/10 in the semantic differencial scale, their Dn score was 12 and FD score was 33. An analysis of the pain intensity distribution (not shown) reveals that 12% (N=12) had mild (1-3) pain, 58% (N=58) had moderate pain (4-6), while 30% (N=30) had severe pain (7-10). Also, their level of Dn was as follows: minimum (N=63, 63%), mild (N=21, 21%), moderate (N=12, 12%), and severe (N=04, 04%). 28% (N=28) had minimal FD, 34%(N=34) reported moderate FD, others had 32% (N=32) and 6% (N=6) severe and cripling FD respectively (table 2). Level of Dn significantly (P<0.05) correlated to FD and BMI while pain intensity correlated significantly (P<0.01) with both Level of Dn and FD (tables 2-4, fig. A & B). Age, gender and pain duration did not significantly relate to level of Dn and FD.
|
Variables |
Minimum |
Maximum |
Range |
Mean ± SD |
|
Age(Years) |
20.00 |
85.00 |
65.00 |
54.00 ± 12.84 |
|
Weight(Kg) |
35.00 |
150.00 |
115.00 |
73.89 ±17.73 |
|
Height(m) |
0.96 |
1.90 |
0.94 |
1.64 ± 0.11 |
|
BMI (Kg/m2) |
15.77 |
50.70 |
34.94 |
27.45 ±5.99 |
|
Pain duration (months) |
6.00 |
180.00 |
174.00 |
26.06 ±32.37 |
|
Pain intensity |
2.00 |
9.00 |
7.00 |
5.63 ± 1.84 |
|
Depression score |
0.00 |
37.00 |
37.00 |
12.20± 8.33 |
|
Disability score |
0.00 |
80.00 |
80.00 |
33.40 ± 18.10 |
BMI - Body mass index, Kg – Kilogram, m – metre, m2 – metre squared SD – Standard deviation
Table 1. General characteristics of the respondents and their psycho-physiological variables
*Significant at 0.05 alpha level
Table 2. Chi-square test of association between levels of depression and functional disability in patients with chronic low back pain.
*Not significant.
** Correlation is significant at the 0.01 level (2-tailed).
Table 3. Spearman Rank Correlation Coefficients showing relationship among the studied psycho-physiological variables.
|
Levels of Depression |
||||||
|
BMI Rating |
Mini mal |
Mild |
Moderate |
Severe |
X2 |
p |
|
Underweight (>18.5) |
1 |
3 |
0 |
0 |
18.84 |
0.03* |
|
Normal (18.5-24.9) |
19 |
2 |
2 |
1 |
||
|
Overweight (25.0- 29.9) |
34 |
8 |
5 |
3 |
||
|
Obese (30.0-39.9) |
9 |
8 |
5 |
0 |
||
*Significant at 0.05 alpha level.
Table 4. Chi-square test of association between levels of Depression and Body Mass Index (BMI) of subjects (N=100).
Discussion
Standard internationally accepted definition of chronic pain (CP) is not available (Harshall and Ospina 2003), however IASP defines CP as pain without apparent biological value that has persisted beyond the normal tissue healing time of 1-6months and recommended 3 months as a good cut off point between acute and CP (Merskey and Bogduk, 1994). Also, it is known that most LBP patients who attend physiotherapy clinics are chronic episodic back pain sufferers experiencing a flare-up and who have been on and off chemotherapy and/or physiotherapy (Egwu and Nwuga, 2008). Therefore, no attempt was made in this study to control subject’s therapy.
In this study, the relationship of duration and intensity of LBP with Dn and FD was investigated among patients whose pain had lasted for at least 3months. The result reveals that level of Dn significantly (P<0.05) correlated to FD while pain intensity correlated significantly (P<0.01) with both Level of Dn and FD.
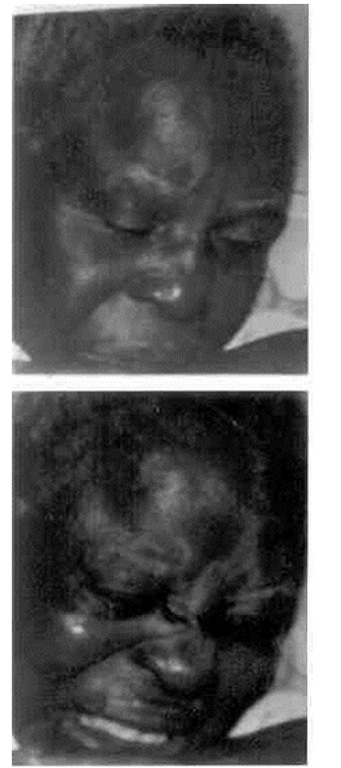
In oder to understand and explain why rise in pain intensity and not the duration of pain affect Dn and function, the ambient mood state, culture and belief system of this cohort need to be clearly understood. Pain is known to have affective, cognitive, emotional and sensory components and it has been observed that majority of Nigerian patients with LBP are in the low-medium socio-economic status and report for treatment late (Merskey and Bogduk, 1994; Egwu and Nwuga, 2008). The reason why patients report late for treatment is believed to be due to the fact that in Africa, pain is culturally interpreted as a harmless experience that accompany ageing (Onyejeme et al, 2002; Egwu and Nwuga, 2008)). Consequently, complaining of pain is seen as a sign of weekness and facial expression of pain is subdued as much as possible (fig. A) until the individual’s tolerance limit is exceeded. This behaviour had been explained by Zola (1973) who observed that people seeking help for a symptom for the first time do so because they are unable to tolerate it any longer. Also, perception of the nature and meaning of incoming sensory information, how the body responds physiologically and what actions are taken, as well as anticipation of what the future holds, are inextricably intertwined (Fordyce, 1995). Further, emotional states influence whether and how an aversive stimulus like pain is perceived. Emotional states also influence physiological processes such as heart rate, blood pressure and muscle tension, which then feed back to colour the perception of what is happening, the meanings assigned to it, the consequences inferred to follow, and the actions taken in response.
Fig. 1. Pain is endured culturally without complain and without facial expression suggesting its presence (fig.A), until the individual’s endurance limit is exceeded (fig.B) before patient finds need to seek help to stop this suffering from rising pain intensity leading to depression and functional disability.
A = pain, B = increased pain intensity
Therefore, the observed corelation between pain intensity, Dn and FD indicate that rise in pain intensity (fig.B) [reflecting the rising ectopic discharge of noxious impulses from nerve irritation enhancing the sinusoidal voltage oscillation in the dorsal root ganglion mambrane potentials] is one exercabating symptom that become intolerable among patient with CLBP driving them from the lower to the higher extremes of the Dn continuum. In addition, pain is known to focus emotions during difficult life situations, and when we assess ourselves in a situation and don’t like where we are, where we have been, or where we are going and we can take no action to close the gap, we consider ourselves as suffering (Budd 1992; Worz 2003). Consequently part of the factors that determine tolerance limit is the feeling of suffering and/or perceived threat to life both of which affect level of Dn and FD. Thus, the level of Dn (minimum – severe) and FD (minimum – cripling) relates to the level of suffering percieved due to the worsening impact of poverty, high number of life stressing events and rising intensity of pain on work, motor activity and social role perfomance until some of the patients become severely(endogenously) depressed and/or crippled (unable to walk properly).
A 4% rate occurance of severe (major) Dn was observed in this study, this is very low compared to reports (16% – 37%) from advanced countries (Sullivan et al., 1992; Banks and Kerns, 1996; Hope and Foreshaw, 1999; Caragee, 2001; Cairns et al, 2003; Currie and Wang, 2003). However, it falls within the prevalence range (1.5% – 57%) according to the diagnostic and statistical manual of American Psychiatric Association (1980). This wide variation in the estimates of MDn is said to be dependent upon the setting, population and diagnostic instrument used.
The reason for this low prevalence of MDn in south-west Nigeria may therefore be related to the high tolerance for pain by an average African and the peculiar Yoruba culture of denial (American Pain Society, 2005; Green et al, 2003). It has been reported that Caucasians report their pain promptly and take more opioids while African Americans with chronic pain report pain late and take less quantity of opioids, have more pain, depression, post traumatic stress disorders and impairment in their physical, emotional and social health (Green et al, 2003, Meldrum, 2003). Thus, based on the theory of stimulus and habituation, they have less likelihood of rating depression as severe (Green et al, 2003; Egwu and Nwuga 2008). Besides, Yoruba culture mixed with christien religion don’t admit or orally express negative emotions. For instance, somebody who is weak or in pain will rather say ‘I am strong’, while somebody who is penniless will say ‘I have too much money’. Consequently, some patients whose Dn may have been of clinical level may have played it down thus explaining the low prevalence of MDn observed in this study.
Group health cooperative centre for health studies (2006) pointed out that there is significant differences among socio-cultural groups in the link between obesity and Dn. They noted that in groups were obesity is more common (low-medium socio-economic status non Caucasians) there is less Dn among obese people because they are not stigmatized. This report is consistent with our current finding that despite a significant relationship between BMI and Dn, non of the 22 obese respondent was severely depressed and it is in tandem with the perception in poor countries that being fat is a sign of wealth (Onyejeme et al, 2002; Haslam and James, 2005).
Conclusion
Pain intensity (not duration) correlate significantly with both level of Dn and FD without age and gender bias. Level of Dn also significantly correlate to FD and BMI with a 4% rate occurence of MDn underscoring the importance of the bio-psycho-social approach to CLBP therapy.