Introduction
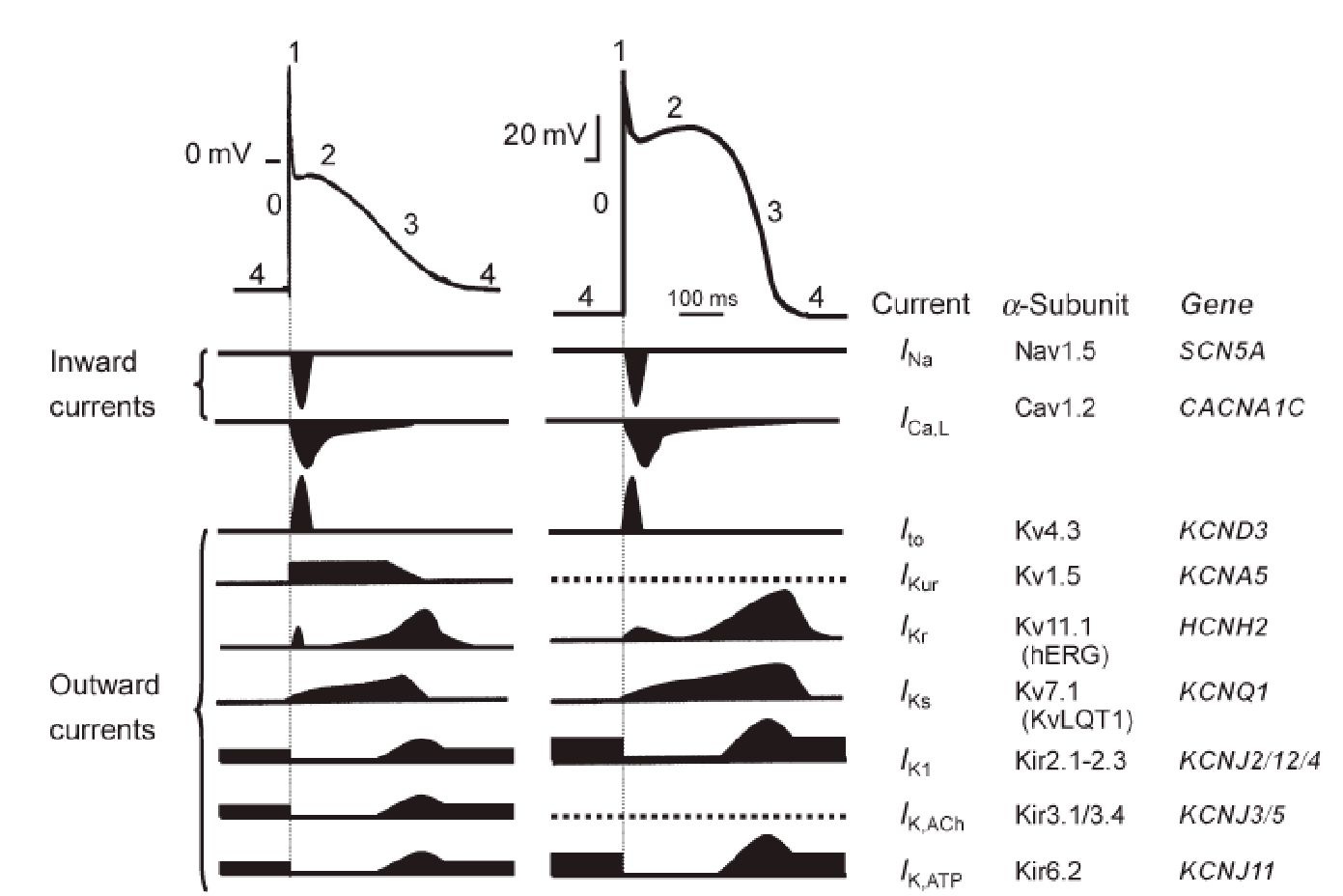
The cardiac action potential is arised by the highly orchestrated activity of dozens of ion channel proteins. These transmembrane proteins govern the influx of ion across the sarcolemma of cardiomyocytes generating the ionic currents responsible for excitation. In order to myocardium contract and ensure rhythmic pump function, the long-lasting action potential of the working myocardium maintains a refractory state. Because some channels must recover from inactivation after-repolarization before they have ability of re-opening, and during this time, the myocardial cells remain refractory for re-excitation. Typical normal action potentials consist of five distinct phases (Figure 1). Na+ influx triggers a rapid depolarization (phase 0) followed by an early fast repolarization phase (phase 1) and a plateau phase (phase 2), in which repolarization is slowed due to the activation of inward Ca2+ current. During the final rapid repolarization phase (phase 3), membrane potential returns to the resting level (phase 4). Therefore, normal action potentials attributed to the normal function of ion channel participated to formation of action potentials.
Fig. 1.Currents of sodium, calcium and potassium channels underlie the atrial and ventricular action potential.
Ion channels in human heart disease
Regular excitation is formed by normal AP which generated in the sino-atrial node and spreads throughout the heart in an orderly manner. Oppositely, disorganization of electrical activity is the basis of cardiac arrhythmias. Arrhythmias are caused by the perturbation of physiological impulse formation, impaired impulse conduction, or disturbed electrical recovery. Abnormal excitability of myocardial cells may give rise to kinds of cardiac diseases.
The most ordinary cardiac arrhythmia diseases was inherited long QT syndrome (LQTS) which was recognized 40 years ago as 2 distinct clinical phenotypes, such as the Romano-Ward and the Jervell and Lange-Nielsen syndromes. Interestingly, while LQTS was initially thought to be a pure cardiac channelopathy, it is now clear that non-ion-channel encoding genes may also cause the desease. Nevertheless, LQTs attributed to dysfunctions of ionic currents, either directly (ion channel) or indirectly (chaperones and/or other modulators). To date, 12 forms of inherited LQTS described because LQTS arise from polygenic causes and 9 of them directly combine with ion channels (Table 1). LQT1, 2, 5, and 6 are referred to prolong the plateau of cardiac APs (phase 2) by reducing K+ channel currents activated during depolarization. LQT1 and 5 are caused by mutations in KCNQ1 (KvLQT1) and KCNE1 (MinK), which encode the a and ancillary P subunits, respectively and together form the slowly activating delayed rectifier K+ current (IKs). LQT2 and 6 are caused by mutations in KCNH2 (human-ether a-go-go-related gene; HERG) and KCNE2 (MiRP1), which encode the a and putative P subunits, respectively and together form the rapidly activating delayed rectifier K+ current (IKr). LQT7 is characterized by mutations in KCNJ2 (Kir2.1), which reduces the inward rectifier K+ channel current (IK1) to slow the return of the membrane to the resting potential. These cause failure of normal inactivation to decrease of K+ current (loss of function) and abbreviate action potentials. Besides potassium channel, LQT3, 10 attributed to mutations in hNaV1.5 (SCN5a), and SCNb4, which encode a and ancillary P subunits of Na+ channel. LQT8 are determined by mutation in CACNA1c, which encode alpha subunit of calcium channel. LOT3,10 and LQT8 arise from the increase of Na+ currents and Ca2+ currents, respectively, for prolong action potential. Therefore, "loss of function" or "gain of function" mutations in the affected ion channels are often formed different phenotypes of cardiac arrhythmia desease.
Except the mentioned above, LQT4,9,11,12 are determined by mutation in ANK2, Cav3, AKAP9 and SNTA1, which encode ankyrin B, caveolin, A-kinase-anchoring protein and alphal1-syntrophin, respectively. All proteins increase or decrease the ironic currents (loss of function or gain of function). Although the remarkable genetic heterogeneity in LQT, three genes, such as KCNQ1 (LQT1), KCNH2 (LQT2) and SCN5A (LQT3), are dominant and cover more than 90 percentage of LQTS patients with identified mutations. With exception of LQTS, some of these involve gain of function mutations in K+ channels (short QT syndrome) and loss of function mutations in and Ca channel and Na+ channels (Brugada syndrome, cardiac conduction disease, etc). Additional congenital arrhythmia syndromes continue to be described, and these are summarized in Table 1.
|
current |
disease |
gene name |
chromosomal locus |
Protein |
functional effect |
inheritance |
|
INa |
LQT3 |
SCN5A |
3p21 |
sodium channel alpha subunit (Nav1.5) |
gain of function |
AD |
|
BrS1 |
SCN5A |
3p21 |
sodium channel alpha subunit (Nav1.5) |
loss of function |
AD |
|
|
AF3 |
SCN5A |
3p21 |
sodium channel alpha subunit (Nav1.5) |
loss of function |
AD |
|
|
PCCD |
SCN5A |
3p21 |
sodium channel alpha subunit (Nav1.5) |
loss of function |
AD |
|
|
SSS |
SCN5A |
3p21 |
sodium channel alpha subunit (Nav1.5) |
loss of function |
AD |
|
|
LQT10 |
SCNb4 |
11q23.3 |
sodium channel beta subunit |
increas sodium channel |
AD |
|
|
ICa,L |
TS/LQT8 |
CACNA1C |
12p13.3 |
calcium channel alpha subunit |
gain of function |
AD/mosaicism |
|
BrS3 |
CACNA1C |
12p13.3 |
calcium channel alpha subunit |
loss of function |
AD |
|
|
BrS4 |
CACNB2b |
10p12 |
calcium channel alpha subunit |
AD |
||
|
Iks |
LQT1 |
KCNQ1 |
11p15.5 |
IKs potassium channel alpha subunit (KvLQT1) |
loss of function |
AD |
|
JLN1 |
KCNQ1 |
11p15.5 |
IKs potassium channel alpha subunit (KvLQT1) |
gain of function |
AR |
|
|
AQT2 |
KCNQ1 |
11p15.5 |
IKs potassium channel alpha subunit (KvLQT1) |
gain of function |
AD |
|
|
AF1 |
KCNQ1 |
11p15.5 |
IKs potassium channel alpha subunit (KvLQT1) |
gain of function |
AD |
|
|
LQT5 |
KCNE1 |
21q21.1-q22.2 |
IKs potassium channel beta subunit (Mink) |
loss of function |
AD |
|
|
JLN2 |
KCNE1 |
21q21.1-q22.2 |
IKs potassium channel beta subunit (Mink) |
gain of function |
AR |
|
|
AF5 |
KCNE1 |
21q21.1-q22.2 |
IKs potassium channel beta subunit (Mink) |
gain of function |
AD |
|
current |
disease |
gene name |
chromosomal locus |
Protein |
functional effect |
inheritance |
|
IKr |
LQT2 |
KCNH2 |
7q35-q36 |
IKr potassium channel alpha subunit (hERG) |
loss of function |
AD |
|
SQT1 |
KCNH2 |
7q35-q36 |
IKr potassium channel alpha subunit (hERG) |
gain of function |
AD |
|
|
AF2 |
KCNH2 |
7q35-q36 |
IKr potassium channel alpha subunit (hERG) |
gain of function |
AD |
|
|
LQT6 |
KCNE2 |
21q21.1-q22.2 |
IKr potassium channel beta subunit (MiRP) |
loss of function |
AD |
|
|
AF6 |
KCNE2 |
21q21.1-q22.2 |
IKr potassium channel beta subunit (MiRP) |
gain of function |
AD |
|
|
Iki |
AND/LQT& KCNJ2 |
17q23.2-q24.2 |
IK1 potassium channel (Kir2.1) |
loss of function |
AD |
|
|
SQT3 |
KCNJ2 |
17q23.2-q24.2 |
IK1 potassium channel (Kir2.1) |
gain of function |
AD |
|
|
AF4 |
KCNJ2 |
17q23.2-q24.2 |
IK1 potassium channel (Kir2.1) |
gain of function |
AD |
|
Table 1. Mutations of ion channels
Mechanism of ion channels dysfunction
Based on the discussion mentioned above we can easy to understand the mutation how reduce or increase the currents and lead the kinds of cardiac arrhythmia. The change of the magnitude of currents in cardiac is based on the below three factors. For instance, the total number of channels on the membrane (N), the open probability of the channel (P0) and the conductance of single channel (i). Gain of function or loss of function mutations of ion channel through changing of N, Po and I alone or all contribute to kinds of congenital cardiac arrhythmia.
Change of the channel number
There are two distinct process in which can change the number of channel in the plasma membrane, one is in the synthesis channel process and another is during the channel trafficking.
About defective synthesis of mutations contained the premature termination codons is maybe the most mutations of ion channel. For example, there are one fourths of all mutations of hERG channel (http: //www. fsm. it/cardmoc). The protein encoded by the mutation with premature termination codon is a truncated one which can be eliminated by nonsense-mediated mRNA decay. And the hERG truncation mutation is proved to be clear by the nonsense-mediated mRNA decay in recently.
Exception of the nonsense-mediated mRNA decay, another important clear mechanism is at mRNA level by microRNA (miRNA) mediated mRNA silencing. The degradation of the target mRNA is through partial complementary combination with the miRNA followed binding with kinds of protein or nucleotide to form a huge ribosome. To date, many miRNA are detected in heart and decrease of ion channel protein at translaton or/and transcript levels. There are three steps during the process of ion channel synthesis: i) the formation of core-glycoslyted monomer in ER followed the correct to the tetramer ii), iii) then complex glycaslytaton to form the mature subunit in Gorgi. Accordingly, Western blot check can be utend to detect weather composition of the channel protein is complete. The primarychannel protein is common synthesized in ER.
In order to export completely from the synthesis location (ER), each channel subunit protein contained more than one of the ER exit signal (D/E-X-D/E) motif which can guide the protein correctly from ER to Golgi, where X represens any kinds of amino acid. To ensure the channel deviated from ER, channel form a tetramer in ER by masking or shielding the ER retention signal. Therefore, mutations in ER exit signal or with correlation of the assembly of channel maybe lead to the retention in ER then decrease the number of channel in the membrane.
Change of channel open probability
Change of activation and inactivation maybe are two ways of altering of channel open probability. In Xenopus laevis oocytes system, to date many mutations have been detected to alter the channel gated. But there are much difference between the oocytes system and the mammalian system. In addition, there are many mutations that have been expressed in mammalian and shown to result in gating defects.
Change of single channel conductance
To alter the conductance of single channel, the mutation sites of ion channel exits in the vicinity of the selective filter. Owing to the selective filter of ion channel is determined the kinds of ions across the channel. Accordingly, the single channel conductance change may be attributed to the conformation altering of the selective filter.
Sodium channel
Cardiac voltage-gated sodium channel has critical role in excitability of myocardial cells and proper conduction of the electrical impulse within the heart. Infux of Na+ across sodium channel is responsible for the initial fast upstroke of the cardiac action potential. Therefore, this inward sodium channel triggers the initiation and propagation of action potential throughout the myocardium. The gene of SCN5A encodes the major sodium channel in heart.
Structure of sodium channel
The voltage-gated sodium channel is composed by a pore-forming a subunit and an ancillary P subunit. Nav1.5 encoded by SCN5A consists of four homologous domains (D I -DE) and each domain has six transmembrane segments (S1-S6). Similar to other voltage-gated ion channel, the S4 contained many positive residues in each domain forms the voltage sensor and the S4 and S5 in all domains together make up ion-conductance pore including the selectivity filter. When sodium channel is activated, influx of Na+ begin, thereby the depolarizing of the membrane until the activation of L-calcium channel, at last forming the upstroke of action potential. Continue to depolarization, the fast and low inactivation happen causing the sodium channel close. Sodium channel gating properties and current kinetics may be altered when channel is dysfunction.
Cardiac sodium channel function can be regulated by a vast number of proteins. The single tansmembrane |3-subunit consists of a small C-terminal cytoplasmic domain and a large glycosylated N-terminal extracellular domain. The ancillary subunit alters the currents density and kinetics by physical interaction with the a subunit. Other proteins regulating Nav1.5 by directly binding include ankyrins, fibroblast growth factor homologous factor 1B, calmodulin, caveolin-3, Nedd4-like ubiquitin-protein ligases, dystrophin, and syntrophin, as well as glycerol-3-phosphate dehydrogenase 1-like protein and MOG1. In addition, sodium channel density and kinetics are furthermore also regulated by phosporylation and glycosylation, even by changes in temperature.
Functions of sodium channel in heart
During myocardial ischemia, the mechanisms involved in arrhythmogenesis are complex, but excitability and conduction are considered as the major determinants. During ischemia, local metabolic changes within the myocardium lead to inactivation of the sodium current and consequent repression of cardiac excitability and slowing of conduction. In clinical, slowing conduction produced by sodium channel blockers application has been shown to be proarrhythmic. Some papers have reported an association between SCN5A loss-of-function mutations and the occurrence of ischemia-induced severe episodes of ventricular tachyarrhythmias.